Clinical Features of Multiple Myeloma
Clinical Features of Multiple Myeloma
Multiple myeloma (MM) is a lethal haematological malignancy with an incidence of 40–60 per 1,000,000 per year. The tumour cells are malignant plasma cells of the same clonal origin, and secrete high amounts of monoclonal antibody, known as the M-component. MM is usually preceded by an age-dependent pre-malignancy called monoclonal gammopathy of undetermined significance (MGUS), which is present in >2% of adults over 50 years of age. At diagnosis, MM is characterised by having a high intramedullary tumour-cell content (>10%), osteolytic bone lesions and/or an increasing tumour mass. Progression of intramedullary myeloma is associated with increasingly severe secondary features (lytic bone lesions, anaemia, immunodeficiency and renal impairment) and also, in a fraction of patients, the occurrence of tumour cells in extramedullary sites, such as the blood, pleural fluid and skin. Historically, the prognosis of MM patients has been unfavourable, and to date no patients have been cured. In order to further improve the treatment of MM patients, new individualised treatment strategies are needed, ideally based on new knowledge of the pathogenesis of the disease.
The Cancer Stem Cell Model
One approach for obtaining new knowledge of the pathogenesis of MM is the cancer stem cell (CSC) hypothesis. This hypothesis has gained acceptance in recent years as a model to explain certain aspects of cancer biology. Like organ tissue stem cells, CSCs are thought to be rare and to enter the cell cycle infrequently.1 Furthermore, CSCs are expected to be able to self-renew, thereby maintaining the CSC population, as well as differentiating into different cell types in the tumour, sustaining and reforming the tumour. This implies that CSCs are relatively resistant to therapies designed to target cycling cells, thereby surviving therapy; this means that the tumour can reform after the end of therapy, leading to disease recurrence.1 The first documentation of the existence of CSCs was in acute myelogenous leukaemia (AML) in 1997 by John Dick and co-workers. Using the non-obese diabetic (NOD)/severe combined immunodeficiency disease (SCID) mouse model, a CD34+CD38– cell fraction representing 0.1–1% of the leukaemic cell population was shown to contain the leukaemia-initiating cell or leukaemic stem cell (LSC). In other fractions, only clonogenic leukaemia progenitors were found, and these were unable to regenerate the tumour after serial transplantation in mice.2 The presence of a CSC has now also been indicated in other cancer types, such as breast cancer,3 brain tumours4 and, recently, lung cancer.5
Even though a candidate CSC in MM (MMCSC) has not yet been identified, considerable information has accumulated over the past few years indicating that such a cell population could be present in MM. The low proliferation capacity of MM tumour cells is one of the main arguments for the existence of a precursor entity in MM. This is observed as low bromodeoxyuridine (Brdu) incorporation, with fewer than 0.5% plasma cells incorporating the Brdu, except in advanced disease.6 Combined with the phenotypic heterogeneity reported in MM, this has led investigators to identify a proliferative, pre-plasmablastic cell with self-renewal capacity. However, to clearly demonstrate the presence of a CSC in MM it will be necessary first to identify the clonotypic population of interest, second to demonstrate that this population is capable of reforming the myeloma hierarchy and finally to show that the cells are able to self-renew.
Insights from Normal B-cell Development
There are four biological hallmarks of normal B-cell development:
• rearrangement of the heavy chain;
• rearrangement of the light chain;
• somatic hypermutation; and
• class switching.
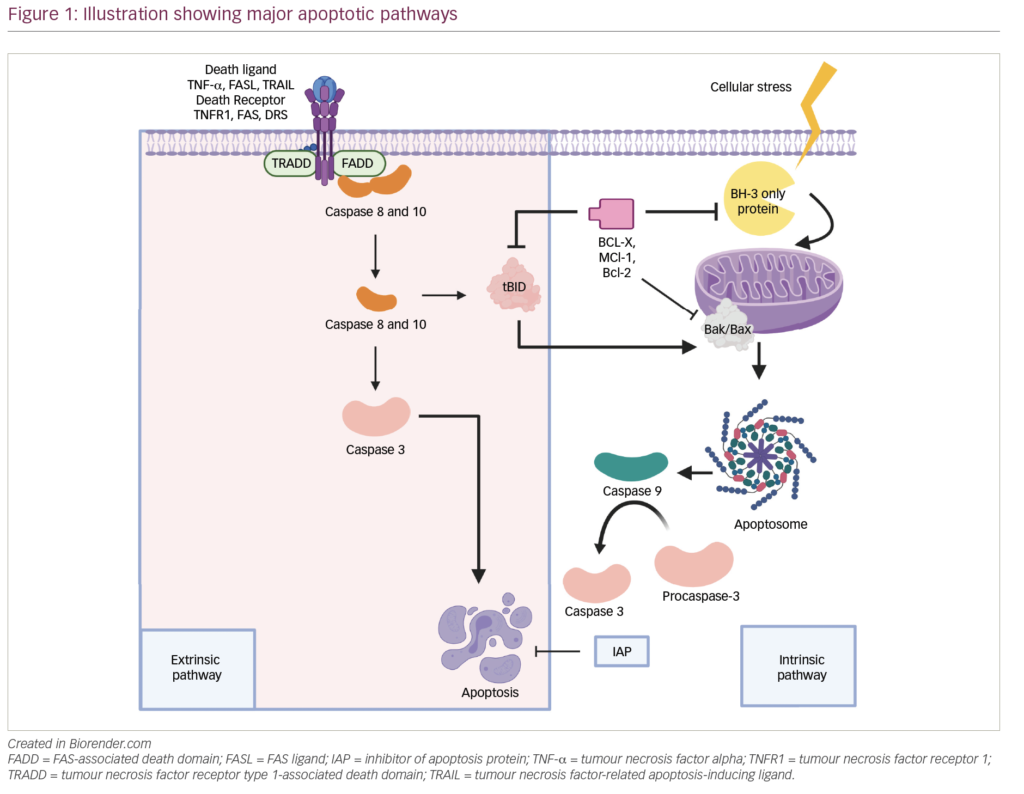
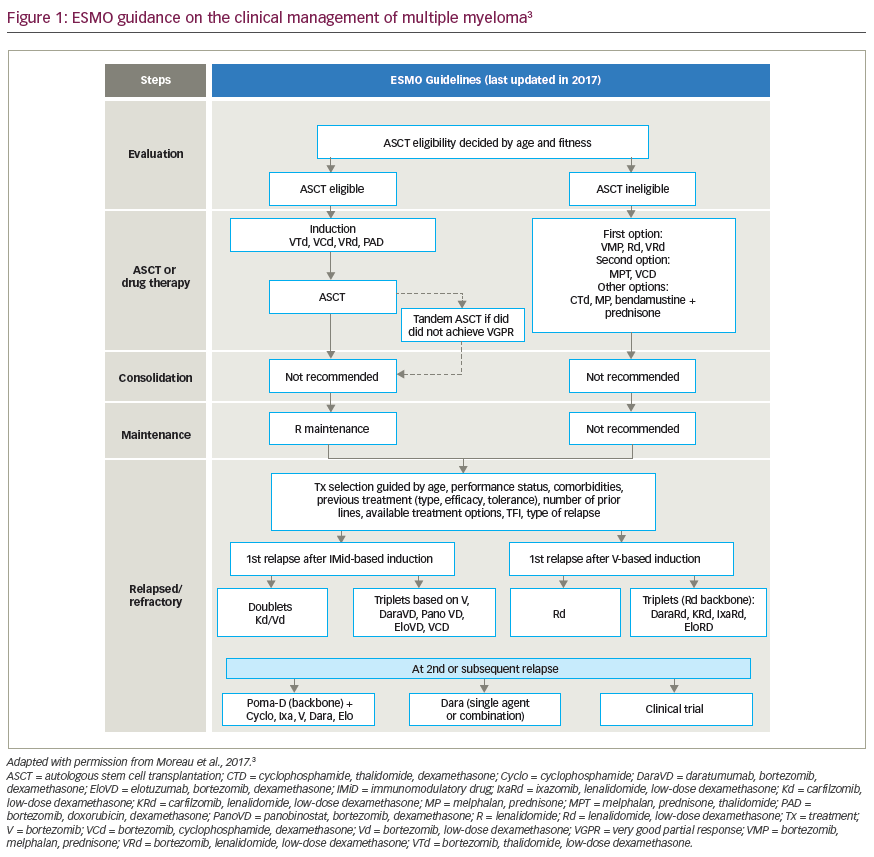
The initial rearrangement of the heavy and light chains is characteristic of pre-B cells and B cells, respectively, and takes place in the bone marrow as part of early B-cell development. However, somatic hypermutation and class switching take place in the germinal centre of the lymph node after antigen recognition.7 Interestingly, rearrangement of the immunoglobulin light and heavy chains as well as somatic hypermutation can be found in the malignant plasma cells.8–10 This indicates that the malignant plasma cells in MM have undergone normal B-cell development and are exposed to the same biological control as their normal counterparts, and that the malignant plasma cell is derived from a post-germinal B-cell type. We believe that there are two possibilities: the MMCSC will be found either in the malignant plasma cell compartment itself or in an earlier B-cell differentiation step (see Figure 1).
Evidence for the Presence of a Multiple Myeloma Cancer Stem Cell
Two characteristics describe the CSC: self-renewal and differentiation to tumour cells. An early study by Hamburger and Salmon11 showed that cells from bone marrow aspirates from myeloma patients were able to form colonies in vitro displaying the phenotypic traits of plasma cells.11 Furthermore, clonogenic growth occurred at a frequency of one in 100–100,000 cells.12 Colonies were established from 86% of the patient samples and the majority of these cells contained monoclonal immunoglobulin in the cytoplasm that was identical to the type found in the patient’s serum or urine.11 Similar findings were reported in a later study by Matsui et al.13 It is therefore likely that cells capable of self-renewal and differentiation are present in MM. However, a candidate CSC still remains to be identified based on surface markers, as was the case for AML.
As mentioned above, there is some evidence that a CSC in MM should be isolated from an earlier B-cell stage than the plasma cell, as so-called clonotypic B-cells have been identified in the peripheral blood of MM patients that have the same rearrangement of the immunoglobulin heavy chain as the malignant plasma cells.14–18
A few groups have looked into additional markers. Rasmussen et al.18 suggested that a clonal hierarchy was present in MM. In peripheral blood, they identified three clonotypic subpopulations from ‘immature’ CD19+/CD38–, expressing immunoglobulin G (IgG) or IgA, to more mature populations of CD19+CD38+ and CD19+/CD38++ expressing IgA only – all with expression of the initial translocations and oncogene activation. Furthermore, clonotypic memory B cells were found in the peripheral blood of 70% of the patients post-transplantation, with a frequency of 0.1% in the memory B-cell population.19
In another line of investigation, Matsui et al.13 divided patient samples into CD138– or CD138+ cells. The CD138– cells were found to have colony-forming potential and to be able to differentiate into CD138+ cells. Furthermore, the results indicated that the colonyforming CD138- cells were positive for CD19, CD45 and CD22. In line with these results, Billadeau et al.9 found clonotypic B-cells in the CD38–/CD45+ population with pre-switched immunoglobulins IgA and IgM.
Although the clinical significance of the presence of clonotypic CD19+ cells is unknown, it is worth noting that these clonotypic cells are present in the peripheral blood of patients after systemic therapy (reviewed in reference 12). Therefore, it would be interesting to look further into subpopulations of the CD19+ cells from the peripheral blood of MM patients, as it might be possible to identify a stem cell candidate here.
Direct evidence for the presence of an MMCSC is still missing, as experiments showing self-renewal as well as tumour-regeneration capacity of a cell type with well-defined markers is still lacking. This would require experiments similar to those described for AML. However, based on knowledge from previous published studies, the odds are in favour of being able to identify an MMCSC within the CD19+ fraction of the peripheral blood. Consequently, a European consortium of scientists called the Myeloma Stem Cell Network (MSCNET) was established in November 2006 as a translational programme to identify and target the myeloma stem cell. The network is supported by the EU’s Sixth Framework Programme and has formulated a strategy that includes genomic and proteomic approaches to examine the nature of the cell underlying MM disease origins and progression.
Perspectives
If the hypothesis of an MMCSC is accepted, two main considerations in patient treatment are evident. First, with the use of autologous transplants there is a high risk of infusing the MMCSC to the patient; therefore, methods should be developed that remove the CSC from the transplant.20 Second, a new therapy should be developed that not only eliminates the malignant plasma cells that cause the symptoms but also targets the MMCSC populations.21 Finally, the presence or absence of the MMCSC after treatment might be a new tool in evaluating the effect of a treatment, as well as redefining remission and the prognosis of the patient. ■