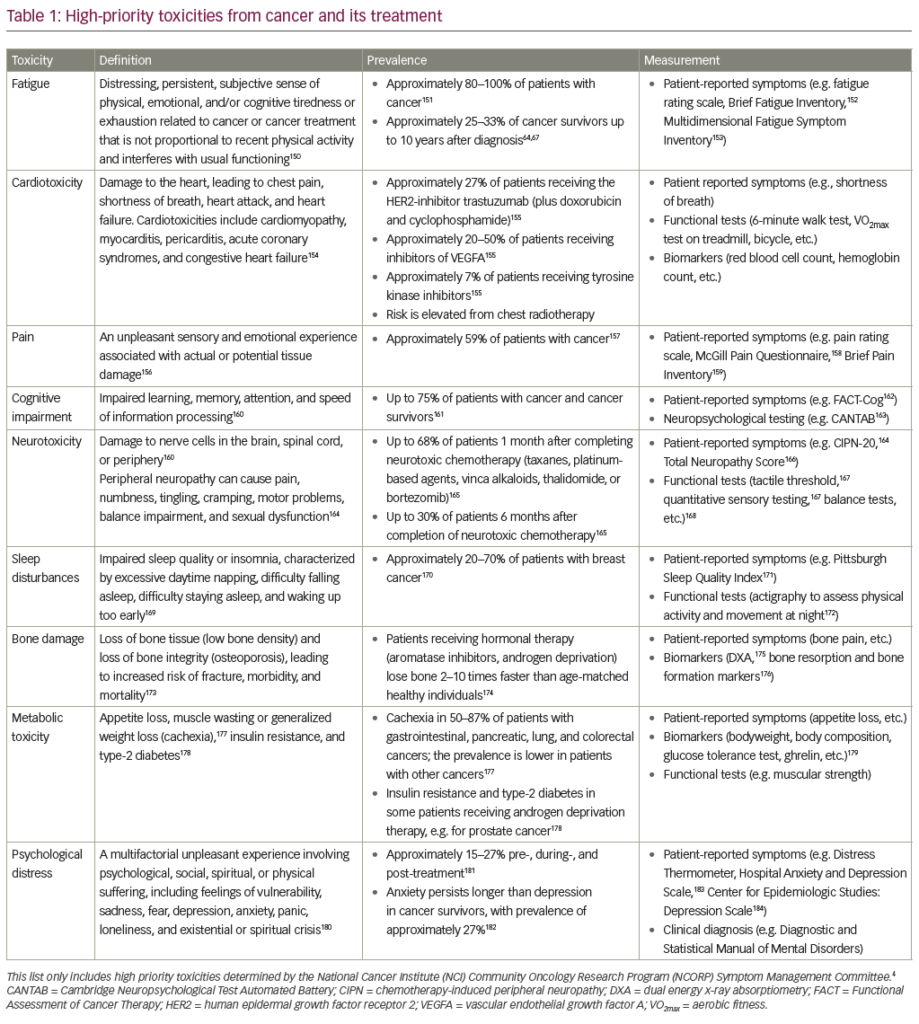
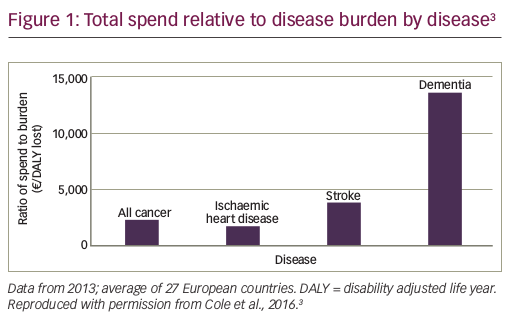
Pain is a common feature of cancer that presents a significant clinical challenge. The prevalence of pain increases as the condition progresses1 and it affects over 80 % of patients with advanced disease.2 Opioids remain the best front-line treatment for providing pain relief (PR), but even when these agents effectively control background pain, patients often experience breakthrough cancer pain (BTcP).3 This may be defined as ‘a transient exacerbation of pain that occurs either spontaneously, or in relation to a specific predictable or unpredictable trigger, despite relatively stable and adequately controlled background pain’.4
BTcP is a heterogeneous entity that varies both between individuals and within individuals over time.5 In a recent study that enrolled 1,000 European oncology patients, the median number of BTcP episodes was three per day, with >95 % of subjects rating the intensity of pain as either ‘moderate’ or ‘severe’.6 Median time to peak intensity was 10 minutes, and the median duration of episodes was 60 minutes.6 The negative effect on quality of life can be significant, as a result of personal suffering and interference with the activities of daily living.6
BTcP may be classified as either spontaneous pain (episodes are unpredictable and not related to an identifiable precipitant) or incident pain (episodes are related to a specific identifiable precipitant).4 There are three sub-classifications of incident pain: volitional (brought on by a voluntary act such as movement), non-volitional (brought on by an involuntary act such as coughing) and procedural (related to a therapeutic procedure such as wound dressing).4 Episodes of pain that occur shortly before the administration of ‘around-the-clock’ (ATC) opioid analgesics (‘end of dose failure’) should not be regarded as BTcP, since the background pain is not controlled in this situation.
This review article summarises the available data on a new fast-acting fentanyl formulation for treating breakthrough pain, which has been developed to accelerate absorption of fentanyl and reduce the time to onset of analgesia.
Management of Breakthrough Cancer Pain
There is currently no ‘gold standard’ for the pharmacological symptomatic treatment of BTcP, but the most common strategy is the use of supplemental analgesia, or ‘rescue medication’.4 The ideal rescue medication should not only be safe and effective, but also have a rapid onset of action, a relatively short duration of effect7 and be suitable for use both reactively (i.e. at the onset of pain) and prophylactically (i.e. prior to the onset of pain in patients with predictable incident pain). These properties would enable BTcP to be rapidly controlled, while avoiding opioid accumulation and minimising adverse effects.8 Currently, BTcP is widely treated with supplemental doses of oral opioids – often immediate-release formulations of morphine. The time to onset of analgesia for these agents is 20–30 minutes, and the time to full effect 60–90 minutes.4 This is not ideal for managing many BTcP episodes.
The requirement for an agent with a faster onset of effect led to the development of transmucosal formulations of fentanyl citrate. Fentanyl is well suited to transmucosal administration because it is highly lipophilic.9 Currently available formulations include oral transmucosal fentanyl citrate (OTFC), fentanyl buccal tablet (FBT), orally disintegrating tablet (ODT), fentanyl buccal soluble film (FBSF), intranasal fentanyl spray (INFS) and fentanyl pectin nasal spray (FPNS). Randomised controlled trials have shown that these formulations can produce analgesia within 15 minutes, and are generally well tolerated.10–15 Recent recommendations published by the European Association for Palliative Care state that ‘BTP can be effectively managed with oral, immediate-release opioids or with buccal or intranasal fentanyl preparations. In some cases the buccal or intranasal fentanyl preparations are preferable to immediate-release oral opioids because of more rapid onset of action and shorter duration of effect’.16
A continuing area of concern with transmucosal fentanyl formulations is that aberrant drug-related behaviour is likely to emerge in about 10 % of patients,17 so continuous monitoring is required. It is generally agreed that the best approach to this problem is not by limiting the availability of these agents, but by the proper assessment and management of both pain and addiction.18
A New Formulation
The conventional approach to tablet formulation is to distribute the active ingredient uniformly throughout the whole tablet, which means that the total dose is not available until the tablet has completely dissolved. In the context of BTcP, the rapid onset of effect is of paramount importance, and a new formulation of sublingual fentanyl citrate tablet (FE tablet) has been developed with the aim of accelerating absorption. It has a unique three-layer structure with a neutral central core surrounded by the fentanyl citrate layer (see Figure 1). This, in turn, is surrounded by an alkaline outer buffering layer, which provides the optimal pH for dissolution and subsequent absorption (see Figure 2). Following dissolution of the surface layer, the total dose of fentanyl is rapidly available, in contrast to a conventional tablet, where the whole amount of fentanyl will only become available after complete dissolution.
The small triangular FE tablet has a neutral taste [data on file]. In vitro testing has shown that it takes approximately 10 minutes for 80 % of the FE tablet to dissolve compared with approximately 1 hour for the OTFC lozenge (Actiq®; see Figure 2; data on file). Six dosages are available: 67, 133, 267, 400, 533 and 800 μg. The tablet is placed under the deepest part of the tongue and allowed to completely dissolve without chewing or sucking. Any remnants may be swallowed after 30 minutes. The optimal dose is determined by upward titration on an individual patient basis, with a maximum of two tablets for each BTcP episode. The range of dosages allows dose escalation in 133 or 267 μg increments until adequate analgesia is achieved. Once an appropriate dose has been established, this should be administered for subsequent BTcP episodes, up to a maximum of four doses per day. If the response to this dose changes markedly, it may be increased or decreased by one increment to maintain an optimal effect.
Pharmacokinetics
The pharmacokinetics of the new FE tablet have been investigated in four phase I trials in healthy adult volunteers under fasting conditions.19–22 The OTFC lozenge was selected where an active comparator was required, as this product has been on the market for the longest period of time.
Dose-proportionality
A drug is said to be dose-proportional if its concentration (usually in plasma) at any given time is proportional to the dose administered. This property is of clinical importance in predicting the effect of dose adjustments, because it means, for example, that doubling the dose will double the plasma concentration. Drugs that lack dose-proportionality are more difficult to use, particularly if the therapeutic window is narrow.
The dose-proportionality of three different doses (133, 400 and 800 μg) of the FE tablet has been investigated in an open-label, randomised, three-way crossover, six sequence, dose-proportionality study.19 Thirty-three subjects were included in the statistical analysis. They received a different single dose on each of three occasions and were then followed up for approximately 2 days, with a 14-day washout phase between doses. Blood samples were collected at various time intervals up to 36 hours after dosing, and the plasma concentration of fentanyl determined using a validated liquid chromatography– tandem mass spectrometry (LC/MS/MS) method. From the area under the plasma concentration-time curve (AUC) (see Figure 3), pharmacokinetic parameters including AUC0-t, AUC0-t’, AUC0-inf and the maximum concentration (Cmax) were then derived. Analysis of these parameters and a linearity analysis performed using a regression approach, demonstrated that these three doses have linear and doseproportional pharmacokinetics after single-dose administration.19
Comparative Bioavailability
Bioavailability is defined as the fraction of an administered dose that reaches the systemic circulation. By definition, the bioavailability of a drug administered intravenously is therefore 100 %, and when administered by other routes is generally less, owing to factors such as incomplete absorption and first-pass hepatic metabolism. If graphs of plasma concentration against time are plotted for the same drug administered intravenously and orally, the bioavailability of the oral drug is the ratio of the oral AUC to the intravenous AUC.
Based on pilot studies indicating a suprabioavailability of the FE tablet over OTFC by a factor of 1.5, the bioavailability of a single 133 μg dose of the new formulation has been compared with that of a single 200 μg dose of the OTFC lozenge in an open-label, randomised, two-way crossover study.20 Forty-four subjects were included in the statistical analysis. They received a single dose of one or other agent on two occasions, separated by a 7-day washout phase, and were then followed up for approximately 2 days. Blood samples were collected up to 30 hours after dosing, and pharmacokinetic parameters calculated as in the previous study. The two agents were found to be bioequivalent, but the FE tablet showed faster absorption and higher early exposure, confirming the suprabioavailability of the FE tablet over the OTFC lozenge by a factor of 1.5. The absolute bioavailability of the OTFC lozenge has been reported to be approximately 47 %,23 so based upon the 1.5 ratio mentioned above, the absolute bioavailability of the FE formulation was estimated to be approximately 70 %.20 The study was repeated in 44 subjects (41 included in the statistical analysis) using single FE doses of 800 μg and single OTFC doses of 1,200 μg, but with a 14-day washout phase.21 Again the two agents demonstrated bioequivalence, but the time to maximum plasma concentration (tmax) of the FE tablet was less than that of OTFC (0.8 hours versus 2 hours; see Figure 4), demonstrating faster absorption. At these higher dosages, both formulations appeared to be safe and well tolerated by the healthy volunteers.21
Dwell Time
In order to evaluate the effect of dwell time (10 and 20 minutes) on the bioavailablility of the 133 μg FE tablet, and to compare it with that of a 200 μg OTFC lozenge, an open-label, randomised, three-treatment, three-way crossover, single-dose study was undertaken.22 The study consisted of three periods with a washout phase of 7 days between consecutive periods. Subjects (n=45) had to: i) let the FE tablet dissolve in the sublingual space for 10 minutes before swallowing the remainder, ii) let the FE tablet dissolve in the sublingual space for 20 minutes before swallowing the remainder or iii) move the OTFC lozenge around in the mouth, and avoid swallowing until it had dissolved. Blood samples were collected at various time-points up to 30 hours after dosing, and pharmacokinetic parameters calculated as before. It can be seen in Figure 5 that the plasma fentanyl concentration produced by the FE tablet during the first 30 minutes with both dwell times was higher than that produced by the OTFC lozenge. The AUC from 0 to 30 minutes for the FE tablet was approximately three times and approximately four times that of the OTFC lozenge for the 10 and 20 minute dwell times, respectively.22
Clinical Application
The FE tablet is indicated for treating BTcP in patients whose chronic background pain has been adequately controlled for at least 1 week by a stable dose of opioids (at least 60 mg of oral morphine/day, 25 μg of transdermal fentanyl/hour, 30 mg of oxycodone/day, 8 mg of oral hydromorphone/day or an equianalgesic dose of another opioid). Efficacy and safety have been evaluated in a prospective, multicentre, randomised, double-blind, crossover study that compared the FE tablet to placebo in 73 opioid-treated cancer patients (from 91 enrolled) who were experiencing one to four BTcP episodes per day.24 First, an open-label titration period identified the optimal dose of the FE tablet for each patient (one of five doses ranging from 133 μg to 800 μg), i.e. one which provided adequate PR for two consecutive BTcP episodes with an acceptable level of adverse events (AEs). Patients were then randomly assigned to the double-blind, crossover second phase of the study to receive one of 13 specified sequences of nine tablets (six FE at the identified optimal dose and three placebo) to be taken for successive BTcP episodes. If satisfactory PR was not obtained after 15–30 minutes, patients were allowed to use their usual rescue medication. Pain intensity (PI) and PR were recorded using an 11-point Numeric Rating Scale (NRS) and a 5-point NRS, respectively, at 3, 6, 10, 15, 30 and 60 minutes after placing the tablet in the mouth. Patient diaries were used to collect these data, as well as the use of any rescue medication.
The primary endpoint was the sum of PI differences at 30 minutes (SPID 30). Secondary endpoints included SPID, PI difference (PID) and PR at all time intervals; SPID at 15 and 30 minutes for pain with and without a neuropathic component; and the proportion of BTcP episodes with reductions in PI scores of >33 % and >50 % at 15 and 30 minutes.24 Safety was monitored throughout the study by regular assessment (i.e. full physical examination and vital signs) and by recording AEs. At each patient visit, the occurrence of AEs was elicited from the physical examination, patient diaries, spontaneous reporting and non-leading questioning. Any AE that emerged during the trial or – if present at baseline – worsened during the trial, was defined as a treatmentemergent AE (TEAE).24
During the double-blind phase, a total of 436 BTcP episodes were treated with FE and 218 with placebo. The primary endpoint was met: mean SPID at 30 minutes after dosing was significantly greater for the FE tablet than placebo (75.0 versus 52.5; p<0.0001). Significant differences in favour of the FE tablet were also reported for the mean PID and PR scores at each time-point from 6 minutes until the last assessment at 60 minutes (see Figures 6 and 7). In patients whose BTcP had a neuropathic component, the mean SPID was higher at 15 and 30 minutes when treated with the FE tablet, but the differences did not reach statistical significance. The proportion of BTcP episodes with >33 % and >50 % reductions in PI scores was also significantly greater for the FE tablet than placebo. At 15 minutes, the >33 % figures were 58.4 % versus 38.4 % (p<0.0001) and the >50 % figures were 26.7 % versus 19 % (p<0.02). At 30 minutes, the >33 % figures were 71.9 % versus 50.5 % (p<0.0001) and the >50 % figures were 53.3 % versus 36.1 % (p<0.0004). Patients required significantly more rescue medication for BTcP episodes treated with placebo than for episodes treated with the FE tablet (38.4 % versus 17.5 %; p<0.0001). TEAEs were mostly of mild or moderate severity and typical of opioid treatment, including vomiting (5.5 %), nausea (4.4 %), diarrhoea (3.3 %) and somnolence (2.2 %). Of the 77 TEAEs (reported by 27.5 % of the patients), 40 (reported by 8.8 % of the patients) were judged to be related to study treatment by the investigators. There were no reports of respiratory depression, circulatory depression, hypotension or shock.24
Conclusions
At the present time, transmucosal fentanyl formulations are not widely used for the treatment of BTcP in cancer patients, although their pharmacokinetic properties are closely matched to the pain profile of BTcP episodes. Their rapid onset of action provides a therapeutic advantage over immediate-release oral opioids, which may not provide relief until well after the time of peak PI. Pharmacokinetic studies have shown that the new FE tablet produces a steeper increase in plasma concentrations than the OTFC lozenge, and a clinical trial with a design similar to that of studies with other fast-acting fentanyls has confirmed that it provides an onset of PR from 6 minutes after administration onwards, and a lasting analgesic effect for up to 60 minutes. 24