Detection of Primary Tumor
In breast cancer, the word ‘detection’ is most commonly used to mean breast cancer screening, most commonly using mammography. Breast cancer diagnosis involves the characterization of a suspicious mass or imaging finding, and entails tissue sampling to make a definitive diagnosis of cancer versus benign disease. Most primary cancers are detected by physical examination or mammography during screening.1 Mammography is the primary imaging modality for breast cancer screening, detection, and diagnosis.2 Both ultrasound and magnetic resonance imaging (MRI) are important adjuncts to X-ray mammography for diagnosis, characterization, and determination of the extent of breast cancer (evaluation of multifocal or multicentric disease), and are routinely utilized in this role.3,4 Mammography, ultrasound, and breast MRI can all be used to direct tissue sampling by needle biopsy for breast cancer diagnosis. MRI has also shown utility for screening in highrisk women, and was recently incorporated in American Cancer Society (ACS) recommendations for screening in high-risk patients.5
The level of fluorodeoxyglucose (FDG) uptake in primary breast neoplasms reflects the rate of glucose metabolism and has been correlated with known prognostic factors and biologic characteristics such as tumor size, histologic type (higher uptake in ductal versus lobular), tumor histologic grade, and some indices of cellular proliferation (higher uptake with higher levels of proliferation).6–11 Overall, the sensitivity of FDG positron-emission tomography (PET) in detecting primary breast cancer is 64–96 %, specificity is 73–100 %, positive predictive value is 81–100 %, and negative predictive value is 52–89 %,1 but in one large study12 the sensitivity was 57 % for lesions <1 cm compared with 91 % for tumors >1 cm and 25 % for in situ carcinoma. Another study confirmed the relatively poor sensitivity of whole-body FDG PET with small tumors (<1 cm), lobular histologic type, and well-differentiated in situ breast carcinoma.13 As primary breast cancer detection requires the ability to depict occult, non-palpable, small (<1 cm) invasive, and in situ malignant lesions, whole-body FDG PET is not used in primary breast cancer detection. Dedicated breast positron-emission mammography (PEM) units have been developed.14 The advantages of PEM include higher spatial resolution, shortened imaging time, and reduced attenuation compared with whole-body imaging. Early studies demonstrated the feasibility of PEM for detecting smaller breast tumors (reviewed in reference 14), and a recent multicenter trial also suggested that PEM may aid in the detection and characterization of both invasive and in situ breast carcinoma.15 Current limitations for PEM include imaging posterior lesions, variable FDG uptake in small tumors, and false-positive findings from prior biopsy.15,16 Recently, PEM with biopsy capability has been developed and is being tested.17 The clinical data regarding dedicated positron breast imaging devices are still limited, particularly compared with the large amount of data supporting and validating screening mammography and other adjunctive primary breast imaging modalities such as ultrasound and breast MRI. The utility of PEM compared with existing breast imaging methods awaits validation in larger prospective trials before more general acceptance and more widespread clinical use.
Staging at Presentation
The extent of spread at presentation is one of the most important prognostic factors for breast carcinoma.18 Staging is typically divided into locoregional staging (for regional nodes, especially axillary nodes) and distant or systemic staging (for sites beyond locoregional nodes). The role of imaging in initial staging of breast cancer patients should be carefully considered in terms of performance and cost–benefit analysis. For example, the utility in staging asymptomatic patients with early breast cancer for distant metastases at presentation using conventional imaging (CI) has been shown to be very low in a number of studies, with overall prevalence of distant metastasis of under 2.5 %.19–23 The experience of using whole-body FDG PET and PET–computed tomography (PET-CT) in the initial staging of early breast cancer is small, but has also confirmed these findings.24,25 In this population with a low prevalence of disease at distant sites, the false/true-positive ratio is too high (with any imaging modality) to be cost-effective and could lead to many unnecessary additional tests and biopsies. For these reasons, whole-body FDG PET-CT should be avoided in patients with early breast cancer.
Axillary Staging
For all patients with newly diagnosed invasive disease (all stages), the status of the axillary nodes is important for prognosis and determining adjuvant therapy.26–28 For this reason, and since axillary nodes are easily accessible, axillary node status is confirmed following removal and histologic examination. Sentinel lymph node biopsy (SNLB) has gained widespread acceptance over the last 10 years to minimize the invasiveness of sampling axillary modes in patients with early breast cancer (tumor <2 cm on mammography, ultrasound, or breast MR and clinically negative axillae). This procedure spares many patients the morbidity associated with complete axillary lymph node dissection (ALND). The reported false-negative rate of SNLB of 5–10 % (with no false-positives) has contributed to making this the standard method of staging the axilla in patients with early breast cancer.29–31 Many early studies of FDG PET focused on detecting axillary metastases.32–36 However, these studies included patients with more advanced primary tumors, increasing the pre-test likelihood of positive PET. The specificity has been consistently high across studies, ranging from 80 to 100 %.37 In the largest prospective multicenter trial so far, of 360 patients,38 FDG PET was 61 % sensitive and 80 % specific for axillary metastases. Patients who had false-negative PET results had significantly smaller and fewer tumor-positive lymph nodes than true-positive cases. This limitation of FDG PET to detect small-volume axillary disease (micrometstasis, small volume of infiltration, and solitary or few positive nodes) has been confirmed in more recent series of FDG PET for staging axillae in early breast cancer with SNLB as the reference standard.13,39–48 These studies, which have included a larger proportion of T1 tumors, have demonstrated a much lower sensitivity for axillary metastases—as low as 20–40 %—particularly in smaller (ranging from 1 to 15 mm) and fewer positive nodes. Thus, FDG PET-CT is not sufficiently accurate to replace SNLB in patients with early-stage breast cancer. FDG PET-CT may have a role for patients with a higher risk of axillary metastases such as those with locally advanced breast cancer (LABC; stage IIb or higher) (see Figure 1). Due to its high specificity, pre-operative FDG PET-CT may direct these patients to ALND, bypassing SNLB, in the case of positive FDG uptake in the axilla. Ultrasound, in conjunction with fine-needle aspiration, is widely used to evaluate any suspicious or palpaple nodes in patients prior to undergoing SNLB.49–52 FDG PET-CT may be used to complement the ultrasound evaluation in the case of equivocal or negative findings. This approach has been previously suggested but needs to be validated in larger prospective trials.41,43,48,53–56
Extra-axillary Locoregional Nodal Staging
Detection of disease in nodal regions not addressed with ALND, i.e. level III (apex of axilla) and extra-axial locoregional nodes, has important prognostic and therapeutic implications.57,58 Several recent studies have shown the benefit of staging patients with newly diagnosed LABC or inflammatory breast cancer (IBC) with FDG PET or PET-CT.59–63 In patients with large (but not inflammatory) primary tumors, FDG uptake in extra-axial regional lymph nodes, including subpectoral, infraclavicular, supraclavicular, and internal mammary (IM) sites, was present in 7–8 % of patients,61,62 and distant metastases were detected in 10–28 % of patients.24,61–63 These findings led to a change in staging of 18–42 % of patients and a change in treatment plan in 13 % of patients.62 The benefit of staging patients with IBC may be even stronger.60,64,65 A retrospective study of 41 patients with IBC60 showed FDG uptake in extra-axial regional lymph nodes and distant sites in 44 % (n=18) and 49 % (n=20) of patients, respectively, and 35 % of patients (seven of 20) with distant metastasis were unsuspected by CI. FDG PET is also useful in detecting recurrent disease in extra-axillary locoregional nodes in patients previously treated for their primary tumor (see Figure 2).66
Distant Metastasis Staging
Although staging for distant metastases is most commonly performed in patients with advanced breast cancer having undergone primary treatment (and possibly more), it is also appropriate for patients with newly diagnosed LABC.67,68 FDG PET can be helpful in the evaluation for distant metastases in patients who have equivocal CI (CT, ultrasound, bone scintigraphy) findings and in asymptomatic patients with elevated tumor markers. In terms of diagnostic performance, several studies have shown FDG PET to have a relative advantage over CI in the evaluation of distant metastases in previously treated patients.69–81 In a meta-analysis of FDG PET for the evaluation of breast recurrence and metastases, Isasi et al.82 reported a median sensitivity and specificity of 93 and 82 %, respectively, in a patient-based analysis. A common finding in these studies comparing FDG PET with CI for the detection of recurrent disease is that FDG PET detects a significantly greater number (about two-fold) of extra-axial lymph node metastases,63,69–71,78,79 including mediastinanal and IM nodes.66 Bone is the most frequent site of recurrence after treatment for primary breast cancer: nearly 70 % of patients with advanced disease have skeletal metastases.83 Metastases from breast cancer can produce a varied physiologic response in bone; lesions can be osteolytic, osteoblastic, or a mixture of the two. Cook et al.84 were the first investigators to correlate the diagnostic performance of FDG PET and bone scintigraphy with the morphologic appearance of individual skeletal metastases at plain film radiography or CT. They showed that FDG PET was superior to bone scintigraphy in the detection of osteolytic metastases, and bone scintigraphy detected significantly more osteoblastic metastases. Others have corroborated these findings,85–89 leading to the general conclusion that FDG PET and bone scintigraphy are complementary methods for the detection of skeletal metastases in breast cancer patients. In our center, bone scintigraphy remains one of the routine studies in breast cancer metastatic staging, with FDG PET-CT to help clarify staging in the case of difficult or equivocal conventional staging. Evolving data suggest that [F-18]-fluoride PET and [F-18]-fluoride PET-CT may improve skeletal metastasis detection compared with bone scintigraphy90–92 and may play a role in breast cancer skeletal metastasis staging in the future.
The combined PET and CT system (PET-CT) has emerged as a routine method of restaging many oncologic patients.93 Fusion of anatomic and metabolic information generally leads to an increase in diagnostic confidence, as shown in an early retrospective study.94 Several of the large retrospective studies of patients being restaged after primary treatment for breast cancer comparing the diagnostic performance of PET-CT with contrast-enhanced CT alone, PET alone, or side-by-side evaluation of CT and PET are summarized in Table 1.94–101 Fused PET-CT data consistently detected more malignant foci in these studies; however, on patient-based analysis they showed marginal (no statistical difference) improvement in sensitivity and specificity for the detection of recurrences. Improvement in accuracy occurred in evaluation of mediastinal and cervical lymph nodes and the skeleton (increased sensitivity for osteoblastic metastases).96,99,100 Treatment Response
Breast cancer is one of the more responsive solid tumors, and there is an ever-increasing choice of effective systemic therapies for breast cancer.102 Evaluating the efficacy of systemic treatment is an important diagnostic need for breast cancer. The two settings where imaging plays an important role in response to systemic therapy are patients with LABC (undergoing neoadjuvant therapy) and patients with metastatic, stage IV disease.
Locally Advanced Disease
Although neodajuvant therapy, compared with adjuvant therapy, has not been shown to improve survival, it does improve surgical options and provide prognostic information.103 Studies have demonstrated that the extent of residual breast and axillary disease after treatment is prognostic for both disease-free survival (DFS) and overall survival (OS).104–106 Patients demonstrating complete pathologic response (pCR), defined as no residual invasive tumor on histopathology at post-therapy surgery, have improved long-term outcome compared with patients without pCR.104,106 One of the primary aims of neo-adjuvant therapy is therefore to assess the response of the primary tumor to the treatment regimen.103 Size-based approaches such as physical exam and mammography have trouble distinguishing pCR from other responses.104,107 This is therefore a role where functional imaging, with its ability to serially quantify metabolic changes in the tumor earlier than morphologic changes, may be particularly helpful. Studies evaluating FDG PET for treatment response in LABC (reviewed in reference 108) have compared standardized uptake value (SUV), a semi-quantitative measure of glycolytic activity, at pre-treatment examination with values at varying times during (early and mid-point), and following completion of treatment (see Table 2). The studies in which the mid-point of therapy was evaluated showed that a drop of approximately 50 % or more in SUV from baseline predicted a good response.109–116 Studies evaluating change in FDG uptake early in the course of therapy (after one or two cycles) suggest that early assessment of response is possible and predictive of subsequent pathologic response.112–119 In a large prospective, multicenter trial of 104 patients with LABC being monitored with FDG PET during neoadjuvant therapy, a threshold of 45 % decrease in SUV after the first cycle of therapy correctly identified 11 of 15 histologic responders and the non-responders with a negative predictive value of 90 %, and similar results were found after the second cycle using a threshold of 55 % relative decrease in SUV.119 The clinical role of FDG PET for evaluating treatment response in LABC is not yet clear, but may be most useful in confirming the lack of clinical response; in this way FDG PET would help avoid ineffective treatment and its adverse effects and decide optimal time for surgery. To use FDG PET for treatment stratification, identification of non-responders with high negative predictive value early during therapy is desirable in order to avoid discontinuation of therapy to patients who might still respond to the full course of treatment. Studies performed after the completion of chemotherapy have shown that although residual FDG uptake predicts residual disease, the absence of FDG uptake is not a reliable indicator of pCR.109,120–122 Breast MR is a more sensitive technique for the detection of residual disease but has relatively poor specificity, with sensitivity of 98 % and specificity of 40 % in differentiating minimal residual from gross residual disease in one study.121 In patients with gross residual disease, post-therapy FDG PET has been shown to complement MRI to help define the extent of residual disease.123 The combination of these two imaging modalities may be the most appropriate approach to guide surgical treatment planning, but it is unlikely to replace histopathologic evaluation for the detection of residual disease. Recent studies have shown that the presence of FDG uptake after therapy is highly predictive of relapse.124 Therefore, even though FDG PET may miss small-volume disease after therapy, the presence or absence of uptake may carry prognostic significance that might help direct the intensity of additional therapy and post-surgery surveillance. Metastatic Disease
Metastatic breast cancer (MBC) is often responsive to systemic therapy and, although cure is rarely achieved, with appropriate therapy, patients often have prolonged survival and improved quality of life. As for the assessment of treatment response of LABC, conventional methods used to assess treatment response in metastases, namely whole-body CT or MRI and bone scintigraphy, can be problematic. Morphologic changes detected at CT or MRI and skeletal scintigraphic abnormalities may persist or be slow to decrease despite good response to systemic therapy and some lesions, especially skeletal, are difficult to measure using standard criteria such as Response Evaluation Criteria in Solid Tumors.125,126 Metabolic imaging with FDG PET has shown promise in making predictions of treatment response or non-response earlier and more accurately than CI. Several small studies evaluating FDG PET for measuring treatment response in MBC have shown, similar to neoadjuvant studies, that significant drops in lesion SUV, typically 40–50 % or more, from pre-therapy baseline can predict responders from non-responders more accurately than CI.127–129 The optimal time-point after initiation of therapy to evaluate MBC with FDG has not been fully determined but may be as early as after the first cycle of therapy. The level of FDG uptake after therapy, again similar to neoadjuvant studies, has also shown to be predictive of outcome in patients completing a course of high-dose chemotherapy.130 A particularly vexing clinical problem for breast cancer clinicians is the evaluation of response of skeletal metastases.131 Changes in bone scintigraphy, the standard method of evaluation of patients with bone metastases, may significantly lag response or even ‘flare’ in response to successful treatment.132,133 The differences seen between bone scintigraphy and FDG PET for bone metastases have led to some investigation into the use of serial FDG PET in assessing bone metastasis response (see Figure 3). In a retrospective study, Stafford et al.134 showed that, in patients with FDG-positive bone-dominant metastatic disease, SUV changes of an index lesion on serial FDG PET correlated with clinical assessment of response and change in tumor marker value. Comparing serial changes in SUV of index lesions to patient outcome measures, Specht et al.135 showed that percentage change in SUV is predictive of time to progression. In this retrospective study, a median decline of 41 % or greater was associated with a longer time to progression.FDG PET-CT is ideally suited for evaluating treatment response of skeletal metastases in breast cancer patients since this technique provides accurate registration of metabolic and morphologic information. Tateishi et al.136 showed, in a retrospective study of 102 patients with breast cancer skeletal metastasis undergoing systemic treatment, that a concomitant increase in CT attenuation and decrease in FDG SUV of the index lesion is predictive of a more durable response to therapy. Larger prospective trials are warranted to confirm these initial observations.
Characterization of Disease
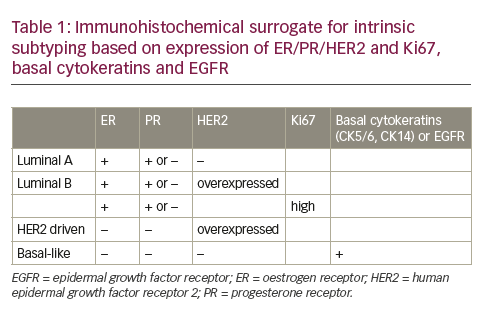
As the array of available treatments for breast cancer increases and therapy is increasingly targeted, there is a growing need to help direct therapy. PET tracers beyond FDG can non-invasively provide quantitative information about in vivo breast cancer biology, helping to direct more individualized therapeutic choices. Preliminary work has focused on several approaches using novel PET tracers, including tumor perfusion and angiogenesis, drug delivery and transport, tumor receptor expression, and early response to treatment in breast cancer (reviewed in reference 137). It is beyond the scope of this article to discuss all of these approaches; however, the ability to image tumor receptors is particularly relevant to breast cancer. Two receptors routinely measured by in vitro assay of biopsy material, both with significant prognostic and therapeutic implications, are estrogen receptor (ER) and HER2. Most of the work to date for breast cancer tumor receptor imaging has been undertaken for steroid receptors using 16 alpha-[18F]-fluoro-17 beta-estradiol (FES).138 This tracer looks promising in preliminary trials because it can identify and quantitatively measure ER heterogenous expression—for example loss of ER expression in metastases arising from ER-expressing primary tumors139,140—and predict response to endocrine therapy.140,141 Likewise, PET imaging approaches for measuring regional HER2 expression in breast cancer also look promising.142
Summary
FDG PET and PET-CT are not sensitive enough to replace the current methods for detection and staging primary breast cancer or for staging the axilla. FDG PET-CT should not be routinely used for the initial staging exam in patients who present with early breast cancer since the prevalence of disease outside the breast and axilla is low and the false-positive/true-positive rate is too high with any staging exam in this group of patients. FDG PET-CT is helpful in staging patients who present with locally advanced and inflammatory breast cancer and for restaging patients who have undergone primary treatment and are suspected of having locoregional or distant recurrence. FDG PET has shown promise in its ability to predict response to systemic therapy both for patients with locally advanced disease receiving neoadjuvant treatment and in the metastatic setting. Finally, advances in PET imaging in breast cancer continue to be made with the use of novel tracers that can help characterize important biologic properties of an individual patient’s tumor and, in this way, direct therapy.