Pathogenesis of Multiple Myeloma
Based on expression array studies, the most important initiation event in MM pathogenesis involves upregulation of D-type cyclins. While cyclin D upregulation may be mediated by reciprocal chromosomal translocations involving the immunoglobulin heavy chain gene such as t(11,14), the mechanism of cyclin D overexpression in other cases remains unknown.4 With time, disease progression is accompanied by additional genetic aberrations such as activation of oncogenes, such as RAS gene mutation or secondary c-MYC translocations, or inactivation of tumour suppressor genes, such as P53 mutation or P18 deletion. Eventually, accumulation of these genetic aberrations confers so much growth and survival advantages to the plasma cells that these neoplastic MM plasma cells no longer require the bone marrow microenvironment for their survival, and clinically may manifest as extramedullary disease such as plasma cell leukaemia.5
Diagnosis of Multiple Myeloma
The diagnosis of MM is based on plasmacytosis (usually >30%) in the bone marrow, osteolytic bone lesions on skeletal survey and the presence of a monoclonal gammopathy in the serum. Therefore, the usual investigations in a case of suspected myeloma include serum protein electrophoresis, bone marrow aspiration and skeletal survey.1 New modalities that enable detection of occult bone disease include magnetic resonance imaging of the bone marrow and positron emission tomography (PET) scan.6 While the detection of a monoclonal immunoglobulin (Ig) in the serum usually raises the suspicion of MM, it is important to note a few points. First, the most common Ig subtypes in MM, in order of prevalence, are: IgG, IgA and then light chain disease. Second, while monoclonal gammopathy is the diagnostic criterion in MM, it may also occur in other lymphoproliferative diseases such as chronic lymphocytic leukaemia (CLL) or indolent lymphoma, or in primary amyloidosis. Apart from clinical symptoms, disease activity is monitored by the level of M-protein.1 Recently, serum free light chain assay has been shown to correlate with the M-protein, and is a useful adjunct to M-protein measurement for the monitoring of myeloma disease, in particular in light-chain MM.
Prognostic Factors
Durie-Salmon versus International Myeloma Staging Systems
An assessment of tumour load is based on the presenting clinical parameters, in which myeloma patients with advanced Durie-Salmon stage fare worse than those with limited stage. However, an international myeloma staging system incorporating diagnostic parameters such as serum albumin and β2-microglobulin levels recently presented a better and more convenient prognostic model than the Durie-Salmon system.2
Biological Factors
The role of karyotypic abnormality is an important factor when predicting clinical outcome. For instance, del(13) is a prevalent aberration and present in about 50% of myeloma patients. Moreover, patients with del(13) had a lower response rate and a shorter survival than those without. Aberrant methylation of gene promoters results in gene silencing and, therefore, tumour suppressor genes may be inactivated by gene hypermethylation.7 For instance, CDKN2B, deathassociated protein (DAP) kinase and SHP1 were found to be frequently methylated in MM, resulting in altered cell signalling. Methylation of DAP kinase, fragile histidine triad gene (FHIT) and secreted protein, acidic, cysteine-rich (SPARC) genes have been shown to confer an inferior survival in small cohorts of patients, and hence may contribute to future risk stratification of myeloma patients.8–11 If verified, methylation may serve as a useful biomarker in risk stratification of MM.
Concerns Regarding Conventional Chemotherapy
Conventional chemotherapy belongs to the alkylator-containing, e.g. MP (melphalan/prednisolone), or the non-alkylator-containing regimens, e.g. vincristine, adriamycin and dexamethasone (VAD).1 MP has been the mainstay of treatment for decades. Subsequent intensification of treatment with additional chemotherapeutic agents such as vincristine, cyclophosphasmide, melphalan and prednisolone (VCMP), vincristine, carmustine (BCNU), cyclophosphamide, melphalan and prednisone (VBCMP) or adriamycin, BCNU (carmustine), cyclophosphasmide, melphalan and prednisolone (ABCMP) has not been shown to be superior to MP following a meta-analysis. However, alkylating agents may compromise the yield of stem cells during stem cell mobilisation, and therefore should be avoided in young MM patients who will subsequently receive autologous HSCT in the course of treatment. On the other hand, the VAD (vincristine, adriamycin and examethasone) regimen does not contain any alkylator, and therefore will not affect the yield of stem cells during stem cell mobilisation. Moreover, VAD induces a rapid response and can be applied in patients with renal insufficiency. Therefore, younger myeloma patients who were eligible for autologous HSCT used to receive VAD as induction therapy while elderly MM patients, who are not eligible for HSCT, may receive MP as first-line therapy until maximal response. However, conventional treatment with MP induces an overall response rate of about 50%, but the complete remission (CR) rate is only 5%.
Historical Treatment Goals with Allogeneic Haematopoietic Stem Cell Transplantation
In young MM patients, the goal of treatment has been to cure the disease, and therefore allogeneic HSCT with stem cell rescue from human leukocyte antigen system (HLA)-identical siblings has been studied in young MM patients. Moreover, any residual disease can theoretically be eradicated by the graft-versus-myeloma effect. However, multiple studies in which MM patients received allogeneic HSCT showed that the treatment-related mortality is excessive (up to 30%).12 Therefore, despite the fact that allogeneic HSCT may be the only modality of cure in MM, the excessive treatment-related mortality has limited its application, and many centres have dropped this modality from the treatment algorithm. Therefore, mini-allogeneic HSCT by virtue of non-myeloablative chemo-irradiation, which will cause lower treatment-related mortality, is currently under intensive research for its efficacy in the treatment of MM.
Recent Advances
In the last decades, one of the most important advances in the treatment of MM is the advent of autologous HSCT (ABMT), which will enable an increase in the rate of CR, and prolonged disease-free and overall survival. However, the procedure is not curative and only results in the prolongation of survival.12 The median survival in MM is about three to five years, depending if the patient has undergone ABMT. The modalities of treatment in patients with MM depend on the age of the patients.
New Agents in Multiple Myeloma – Mechanisms, Safety and Efficacy
Thalidomide and Lenalidomide
In the 1960s, thalidomide was banned as a sedative because of teratogenicity; however, it was approved by the US Food and Drug Administration (FDA) for the treatment of MM in 1998. Clinical trials showed that upfront use of thalidomide plus dexamtheasone results in a high response rate. The major side effects are neuropathy, constipation, bradycardia and venous thrombosis (much less common in Oriental people). Lenalidomide (Revlimid®), a derivative of thalidomide, has been shown to result in a high response rate. However, despite being a thalidomide derivative, the major toxicity of lenalidomide is myelotoxicity rather than neuropathy. Bortezomib
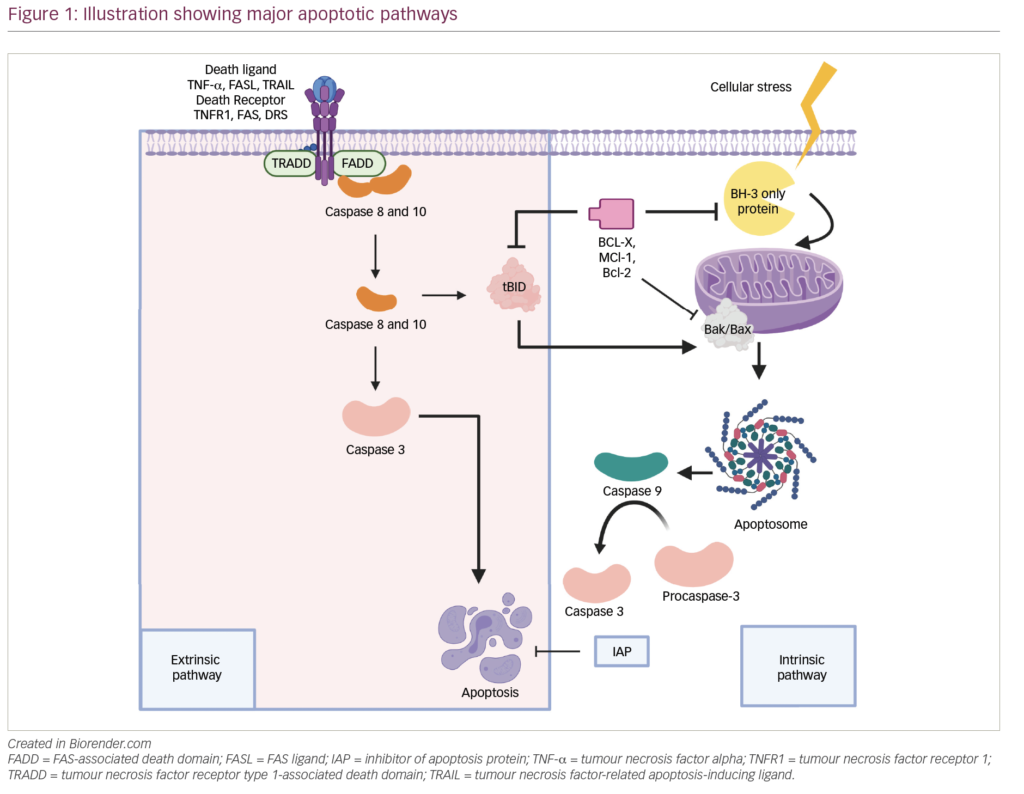
Nuclear factor-kappa B (NF-κB) is a transcription factor that activates transcription of genes that protect MM plasma cells from apoptosis.13,14 However, NF-κB is normally inhibited by IκB by forming a cytosolic complex, thereby precluding nuclear translocation of NFκB and hence transcription of NFκB target genes. In MM, IκB is downregulated by proteosomal degradation, thereby freeing NFκB from the protein complex.13,14 As a result, NFκB is free to translocate to the nucleus and activate transcription of its target genes. Bortezomib, a proteosomal inhibitor that protects IκB from proteosomal degradation, will contain NF-κB in the cytoplasm, thereby preventing activation of anti-apoptotic genes with resultant apoptosis of myeloma plasma cells. Indeed, bortezomib has been shown to be an effective salvage therapy in heavily pre-treated relapsing myeloma patients.15 Moreover, upfront use of bortezomib followed by autologous HSCT results in a high CR or near CR rate of more than 50%, in contrast to the 5% CR rate with conventional chemotherapy alone.16,17 Current efforts are focused on how to optimise therapy to improve the quality of CR, and hence the ultimate goal of cure.
Impact of Targeted Therapy
Upfront use of these targeted therapeutic agents, in particular in combination with conventional chemotherapy, has been shown to increase CR rate from about 5% to up to 30%, which is an unprecedented advance in the treatment of MM. Moreover bortezomib and thalidomide are not myelotoxic, and thus can be used together with myelotoxic chemotherapeutic agents such as melphalan, doxorubicin or cyclophosphamide. Indeed, the thalidomide with MP (MPT) combination has resulted in a CR or near CR rate of about 25% and, importantly, a prolonged survival compared with those receiving MP alone.18 The combination of bortezomib with MP resulted in a CR or near CR rate of about 35%. Similarly, combination of bortezomib with doxorubicin and dexamethasone resulted in a CR or near CR rate of 25%.19 Moreover, in elderly MM patients, treatment used to be of palliative intent only as these subjects are excluded from HSCT. However, as thalidomide and bortezomib are non-myelotoxic, these agents can also be used in elderly patients. Therefore, a decent CR rate may be achieved even in elderly MM patients.
General Treatment Recommendations
Considering the difficulty in achieving CR in myeloma, which is a requisite to cure, the advances in the new therapeutic agents and the survival advantage inherent with bone marrow transplantation, a general recommendation may be devised based on the age of the patient.
Young Multiple Myeloma Patients
Young MM patients, i.e. those <65 years of age, should receive autologous HSCT after initial cytoreduction. Moreover, stem cell collection should ideally be performed at the time of CR or minimal MM contamination of the marrow. Therefore, MM patients receive the bortezomib-containing regimen, which may render a high CR rate prior to HSC collection. There are some studies showing that tandem autologous HSCT may result in superior survival to single autologous HSCT. However, one randomised controlled study showed that patients who achieved >90% response after the first ABMT do not benefit from a tandem ABMT.20 Therefore, the role of tandem autologous HSCT remains to be verified, in particular in the era of targeted therapy. Elderly Multiple Myeloma Patients
Various induction therapies incorporate targeted agents such as MPT or bortezomib with MP (VMP).18 Indeed, in addition to randomised controlled studies that showed a superior CR rate and survival in patients receiving MPT compared with MP, another study also showed superior CR rate and survival in patients receiving MPV than MP.19
Summary
MM is an incurable disease, but major advances in HSCT and novel therapeutic agents have enhanced the CR rate – the pre-requisite to cure. Optimisation of the application of HSCT and targeted therapy will lead to prolonged survival and, hopefully, cure in the future. Moreover, bortezomib may overcome a hitherto unconquered adverse prognostic factor of del(13). Therefore, it is of utmost importance that chromosomal study be performed at diagnosis to risk-stratify the patient. Those with high-risk features may undergo more intensive treatments.