Imatinib (Gleevec®, Novartis Pharmaceutical Corporation, New Jersey, US) is a BCR-ABL1 tyrosine kinase inhibitor (TKI) that has dramatically improved the outcome of patients with chronic myeloid leukaemia in chronic phase (CML-CP).1 Although most of the patients with CML-CP do well under imatinib, approximately 40% of them stop receiving imatinib due to lack of efficacy and/or because of intolerance. In the imatinib arm of the International Randomized Study of Interferon and STI571 (IRIS) trial, 34% of patients were no longer on the study drug at 6 years, for reasons that included lack of efficacy (12%) and the occurrence of adverse events (AEs) (4%).2 Nearly 20% of the patients develop resistance (both primary and acquired),3 and BCR-ABL1 kinase domain (KD) mutations are detected in approximately 50% of patients with treatment failure and progression.4
There are various treatment options available for CML patients who remain refractory to the prior line(s) of TKI treatment.5,6 In patients who fail upfront imatinib therapy, second generation TKIs (2GTKIs; dasatinib, nilotinib and bosutinib) can be administered.7–9 In addition to 2GTKIs, ponatinib (Iclusig®; Ariad Pharmaceuticals, Massachusetts, US) is a potent TKI active against native and mutated forms of BCR-ABL1, including T315I, and it was approved after the phase II PACE study demonstrating that ponatinib was highly active in heavily pretreated Philadelphia chromosome-positive leukaemia patients.10
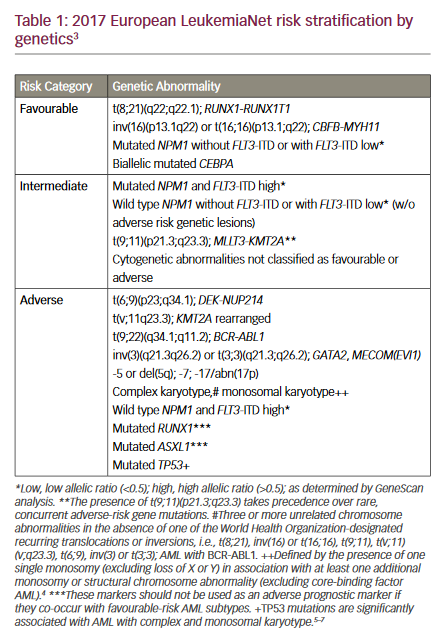
Although having some differences between each other, in the recommendations of European LeukemiaNet (ELN),4 the guidelines of National Comprehensive Cancer Network (NCCN) and European Society of Medical Oncology (ESMO),11,12 there are evidence-based suggestions in order to harmonise the response evaluation and the management of patients with CML both in the upfront and salvage settings.
In this issue of European Oncology and Haematology, Prof Hughes and Prof Saglio summarised the treatment options in patients with CML-CP who failed prior TKIs including alternative TKI treatments and allogeneic haematopoietic stem-cell transplantation (allo-HSCT), and then primarily focusing on a questionnaire which was completed by 14 physicians from different countries.13 The purpose of the questionnaire and the subsequent paper was to understand the perspectives of the CML-treating physicians in the management of refractory CML-CP.
The questionnaire had three sections. In the first section, the consensus responses to four questions mainly focusing on both BCR/ABL1-dependent and BCR/ABL1-independent resistance mechanisms; the difference in the rates of T315I mutation between daily practice and clinical trials; cross-intolerance between different TKIs; and solutions in order to address poor adherence to TKI treatment. The management of AEs, and patient education were also shared.13
In the second part of the questionnaire, the respondents were asked about strategies to combat failure/intolerance to previous 2GTKIs.13 The participants agreed that the chance of achieving a response was much higher in case of intolerance, but patients still have the chance to obtain improved responses after switching to another 2GTKI due to resistance. While choosing another 2GTKI, mutational status and comorbidities of each patient, together with the toxicity profile of the TKI should be taken into consideration.14,15 The respondents also concluded that bosutinib (Bosulif®; Pfizer, New York, US) can be a reasonable treatment modality if there is intolerance to one or more 2GTKI; although, there are some toxicities observed with bosutinib (e.g., diarrhoea) at the dose of 500 mg/day. Additionally, bosutinib has not yet been approved in many countries.
In the second section, the participants were also asked about the role of ponatinib in the management of patients of CML-CP after failing previous lines TKIs. All the participants agreed that a patient with T315I should receive ponatinib regardless of their molecular response.13 Also, nearly all respondents reported that they would not give ponatinib to patients in CML-CP after imatinib failure, unless the patient harbours T315I mutation. But in case of failure to imatinib in a patient with advanced disease, 83% of the participants agreed that ponatinib could be a reasonable choice of treatment.13 Nearly 70% of the respondents agreed that ponatinib could be suitable in patients failing two lines of TKIs; however, there were fewer participants (7/12, 58%) who thought that ponatinib would be an option in patients who had resistance or intolerance to prior two lines of TKI treatments. More than half of the respondents (7/12, 58%) stated that they would not choose ponatinib in the second-line setting in a patient who failed dasatinib or nilotinib as an upfront treatment.
Regarding the role of allo-HSCT, 67% of the respondents agreed that after ponatinib failure, allo-HSCT is the right treatment option.13 Approximately 60% of the physicians would not go for an allograft without trying ponatinib, and all the respondents agreed that allo-HSCT would be appropriate in a patient who is in second CP.13
In the last part of the questionnaire, the consensus responses regarding four questions were displayed.13 The participants revealed that although bosutinib has a limited role in the third- or fourth-lines of TKI therapy, nevertheless, this drug can be still chosen over ponatinib in patients with known risks of cardiovascular events, where there is intolerance to prior TKIs, and in cases who are resistant to two or more lines of TKI treatment without harbouring any mutations.13 In the management of patients who progressed to advanced disease during a TKI treatment, the respondents listed various treatment modalities including the dose escalation of the current TKI, switching to an appropriate TKI, choosing ponatinib in case of T315I mutation, adding conventional chemotherapy to TKI, and allografting in the suitable patient.
Although the management of CML-CP, especially in the newly-diagnosed patient, is generally straightforward, it may vary in the salvage setting, since some of the currently approved TKIs in the management of CML are not available in some countries. This survey in which the management strategies of refractory CML was discussed, does have a value, but obviously has various limitations as concluded by Prof Hughes and Prof Saglio. The new ELN recommendations, which will be published soon, hopefully will address some of the conflicts underlined both in the survey and within this paper, in order to harmonise the management of refractory disease.