Key points
- Olutasidenib induces durable responses in patients with relapsed or refractory (R/R) acute myeloid leukaemia (AML) with isocitrate dehydrogenase 1 (IDH1) mutations in the phase I and II clinical trials.
- The side effects of olutasidenib are well known and highly manageable.
- Olutasidenib represents a therapeutic advance for these patients with a poor prognosis. Olutasidenib received the US Food and Drug Administration’s approval in 2022 for the treatment of adult patients with R/R AML with IDH1 mutations.
Acute myeloid leukaemia (AML) is a rare aggressive haematological malignancy characterized by aberrant differentiation and overproliferation of non-functional myeloid precursor cells that will accumulate in the bone marrow, blood and, occasionally, other tissues.1–5 The prognosis of AML remains poor, especially in older/unfit patients and in the case of patients with relapsed or refractory (R/R) diseases.2,6
Systematic use of next-generation sequencing (NGS) identified recurrent mutations in AML. Among them, mutations in isocitrate dehydrogenase 1 and 2 (IDH1/2) genes are found in around 20% of patients with AML.7,8 IDH mutations are also found in other haematological malignancies, such as myelodysplastic syndromes (MDS) and myeloproliferative neoplasms, as well as in solid cancers, such as low-grade glioma, secondary glioblastoma (80%) and cholangiocarcinoma (8–20%).9–14 They are also associated with clonal haematopoiesis of indeterminate potential.15,16
IDHs are metabolic enzymes that are part of the tricarboxylic acid cycle. They are involved in numerous cellular processes. Several preclinical models provided proof for the oncogenic role of mutant IDH (mIDH). Depending on the cellular context and associated molecular events, they act as either an initiating event promoting transformation or a secondary event that confers selective advantage to the cancer cells. IDH mutations contribute to tumourigenesis through epigenetic dysregulation responsible for the blockade of haematopoietic differentiation, DNA repair impairment and metabolic reprogramming. In preclinical observations, the inhibition of mIDH reverses these alterations and relieves the differentiation blockade, providing strong evidence for the development of mIDH inhibitors. Ivosidenib was the first mIDH1 inhibitor approved by the US Food and Drug Administration (FDA) in 2018 for patients with R/R AML with IDH1 mutations and, in 2019 and 2022, for newly diagnosed (ND) patients with mIDH1 AML unfit for intensive chemotherapy as monotherapy and in combination with azacytidine, respectively.17–19 In 2022, olutasidenib became the second mIDH1 inhibitor approved by the FDA to treat patients with R/R AML with a susceptible IDH1 mutation as detected by an FDA-approved test.20
Normal functions of isocitrate dehydrogenase 1
The IDH family comprises three proteins. IDH1 is located in the cytoplasm and peroxisomes, whereas IDH2 and IDH3 are mitochondrial enzymes.21 IDH1 and IDH2 are metabolic enzymes of the Krebs cycle and have a similar structure. They form homodimers that catalyse reversibly the conversion of isocitrate into α-ketoglutarate (α-KG) while reducing nicotinamide adenine dinucleotide phosphate (NADP+) to NADPH and producing CO2. NADPH is a crucial cellular reducing agent involved in numerous cellular processes, such as glutamine metabolism, lipogenesis, glucose sensing and regulation of cellular redox status to protect the cells against the toxicity of reactive oxygen species (ROS) and oxidative DNA damage.22–24 α-KG is a cofactor for more than 60 α-KG-dependent dioxygenases (α-KGDDs) involved in a wide range of cellular processes, such as hypoxia, angiogenesis, maturation of collagens of the extracellular matrix, DNA repair and regulation of epigenetics.25,26 Hypoxic conditions or altered oxidative metabolism induces an alternative IDH1-dependent pathway, which generates isocitrate and acetyl coenzyme A from α-KG and glutamine.27–29 This alternative metabolism allows biosynthesis and participates in the proliferation of cancer cells.30–32
Isocitrate dehydrogenase 1 mutations and production of D2-hydroxyglutarate
IDH1 mutations have been identified in glioblastoma in 2008 and in AML in 2009.7,12 They are missense mutations leading to the substitution of the conserved amino acid arginine at position 132, which plays a crucial role in the binding of isocitrate to the enzyme’s active site. Among them, IDH1 R132H is the most common in AML. As these mutations are heterozygous, a loss of function and a dominant negative effect of mIDH were initially suspected.33 However, several subsequent studies demonstrated that IDH mutations modify the structure of the active site, reducing its affinity for isocitrate and increasing its affinity for α-KG and NADPH. These alterations lead to the acquisition of a neomorphic enzyme activity that converts NADPH and α-KG into NADP+ and the oncometabolite D2-hydroxyglutarate (D-2HG).34–36
2HG does not participate in any known productive metabolic pathway, and its physiological effect remains poorly understood. This chiral metabolite is physiologically present in tissues in its D- and L-forms at low concentrations that are maintained by 2HG dehydrogenases. The mIDH exclusively produces D-2HG at concentrations 50- to 100-fold higher than those in normal tissues.34–36 D-2HG has a crucial role in the promotion of leukaemogenesis.37 The chemical structures of 2HG and α-KG are highly similar except for a C2 hydroxyl group in 2HG instead of a C2 carbonyl group in α-KG. At high concentrations, D-2HG occupies the same binding pocket as α-KG and acts as a competitive antagonist of α-KG-dependent reactions, inhibiting multiple α-KGDDs.38
Isocitrate dehydrogenase 1 mutations and tumourigenesis
DNA hypermethylation
Epigenetic deregulation is a major mechanism for the development of mIDH AML through inhibition of several α-KGDDs by D-2HG, in particular ten-eleven translocation (TET) 2. Under physiological conditions, TET2 oxidizes 5-methylcytosine to 5-hydroxymethylcytosine, 5-formylcytosine and 5-carboxycytosine, leading to DNA demethylation.39–41 DNA methylation profiling shows that mIDH AML and gliomas are associated with a specific CpG island methylator phenotype characterized by a high degree of DNA hypermethylation in CpG-rich domains.39,42–47 Abnormal DNA hypermethylation has been reported as contributing to cancer formation and tumour progression.48 Of note, cells with TET2 or Wilms tumor 1 (WT1) mutations display an overlapping hypermethylation signature with mIDH1/2 cells, providing an explanation for their mutual exclusion in AML.39,49,50 This epigenetic deregulation modifies the expression of genes involved in cellular differentiation, resulting in a differentiation block with a gene expression profile enriched for genes expressed in progenitor cells.37,39,51,52
Nevertheless, IDH mutations are not sufficient to drive oncogenesis by themselves. In mice models, cooperation between IDH mutations and other molecular alterations, including FLT3 (FMS-like tyrosine kinase 3), NRAS (neuroblastoma RAS) or HOXA9 (Hox-A9) mutations, is required to promote the full transformation of IDH-mutant clones into AML.53–56
Histone hypermethylation
D-2HG increases histone methylation through the inhibition of Jumonji C domain-containing histone demethylases (KDMs), such as KDM4, leading to deficiency in homologous recombination, seemingly making mIDH cells susceptible to poly(adenosine 5′-diphosphate-ribose) polymerase inhibitors.25,51,57,58 In a model of myeloid lineage-specific IDH1 R132H conditional knock-in mice, alteration of histone methylation was responsible for the downregulation of the DNA damage response protein ATM (ataxia-telangiectasia mutated), leading to an age-dependent accumulation of DNA damage in a TET2-independent manner.59 In vitro assays suggested that D-2HG can also directly inhibit the α-KGDD-dependent alkB homologue DNA repair enzymes, leading to the impairment of DNA repair independently of epigenetic deregulation.60
RNA hypermethylation
D-2HG inhibits the α-KG-dependent RNA demethylase fat mass and obesity-associated protein (FTO) that has been described as a promoter of leukaemic transformation.52,61,62 In sensitive wild-type IDH (wtIDH) AML cell lines and primary wtIDH AML cells, FTO inhibition had an anti-leukaemic effect by suppressing aerobic glycolysis, but its significance in the context of IDH mutation AML is still not clear.
Metabolic reprogramming and redox homeostasis shift
Several studies on glioma cell lines and primary cells showed that mIDH affects redox homeostasis by disrupting the NADPH/NADP+ equilibrium, leading to the accumulation of ROS and elevated oxidative stress, possibly in a D-2HG-independent manner.63,64 To counteract this shift in the redox homeostasis, IDH-mutated cells develop a dependency towards the nuclear factor erythroid 2-related factor 2 antioxidative pathway for ROS scavenging.65 D-2HG also inhibits the activity of the branched-chain amino acid transaminase 1 (BCAT1/2), which is known to promote proliferation, survival and stem-cell maintenance in AML.66 The inhibition of BCAT1/2 in glioma cells decreases glutamate levels, leading to cell dependency on glutaminase for glutamate and glutathione synthesis.67 Another study highlighted that IDH1 mutations sensitize tumour cells to hypoxia. A decrease in mIDH1 cell growth under hypoxic conditions was observed, possibly related to an increase in mitochondrial oxidative metabolism dependence and a decrease in glutamine metabolism.68 The accumulation of D-2HG alters also glycolysis and lipid metabolism.69
Dependence on anti-apoptosis proteins
In IDH1 R132H AML cells, D-2HG induces dependence on the anti-apoptotic B-cell lymphoma 2 (BCL2) protein (but not on Bcl-xL [B-cell lymphoma extra large] or Mcl-1 [myeloid cell leukemia 1]) through the inhibition of cytochrome c oxidase in the mitochondrial electron transport chain, leading to the decreased mitochondrial threshold for induction of apoptosis.70 In mIDH1 glioma cells, D-2HG reduces the protein synthesis and the mammalian target of rapamycin (mTOR) pathway, leading to a decrease in Mcl-1 and an increased dependence on Bcl-xL.71 In other tumour cell lines, inhibition of KDM4A by D-2HG led to the activation of the mTOR pathway.72
These contradictory findings highlight that IDH mutations and D-2HG accumulation may have cell- or tumour-type-specific effects. Of note, similar contradictory results have been reported on the influence of D-2HG and hypoxia-inducible factor signalling 1a regulation.33,73,74
In conclusion, IDH mutations and accumulation of D-2HG drive tumourigenesis through several mechanisms from epigenetic deregulation to alteration of DNA repair and a wide metabolic reprogramming. These effects are presumably tumour-type specific. Therefore, the identification of a specific oncogenic process is difficult. Of note, these effects also confer vulnerabilities to tumour cells, bringing potential therapeutic opportunities.
Isocitrate dehydrogenase 1 mutations in acute myeloid leukaemia
The incidence of IDH1 mutations in patients with AML varies from 6 to 16%.75 De novo mIDH1 AML is associated with older age, lower white blood cell count and normal karyotype (NK).7,76–80 NPM1 (nucleophosmin 1) is the most frequent co-occurring mutated gene, followed by DNMT3A (DNA [cytosine-5]-methyltrasnferase 3A) and NRAS.77,79–83 In the context of wild-type NPM1 AML, unfavourable mutations in ASXL1 (additional sex comb-like 1), RUNX1 (runt-related transcription factor 1) and KMT2A-PTD (lysine methyltransferase 2A-partial tandem duplication) genes are frequently associated with IDH1 mutations.80 On the contrary, IDH1, TET2 and WT1 mutations are mutually exclusive.39,49,50
The significance of the prognosis of IDH1 mutations is inconsistent when studied as a single factor.75,76,84,85 However, it seems that IDH1 mutations confer a worse prognosis in patients with NK and wild-type NPM1 but do not affect the favourable prognosis of patients with NK and NPM1 mutations, especially in patients <60 years old. This favourable outcome seems to be abolished by the co-occurrence of DNMT3A or FLT3 mutations.79,80,82,85–87
D-2HG production reflects the neomorphic enzymatic activity of mIDH. The detection of serum D-2HG has a well-established clinical value in patients with AML. At diagnosis, an increased D-2HG concentration is a strong biomarker predictive of the presence of IDH mutations, with great specificity. The lack of normalization of D-2HG levels under treatment is associated with the failure to achieve complete remission (CR) and shorter survival.88,89
Treatment of isocitrate dehydrogenase 1-mutated acute myeloid leukaemia with olutasidenib
Patients with IDHm R/R AML are usually not eligible for intensive chemotherapy which was the only curative treatment until recently. The development of targeted therapies, such as IDH or FLT3 inhibitors, provides new therapeutic options for these patients.
As a proof of concept, the inhibition of mIDH with small-molecule selective inhibitors decreases intracellular D-2HG levels, reverses epigenetic deregulation and releases the differentiation block in vitro and in vivo in preclinical studies, leading to the clinical development of mIDH inhibitors.37,56,90–95
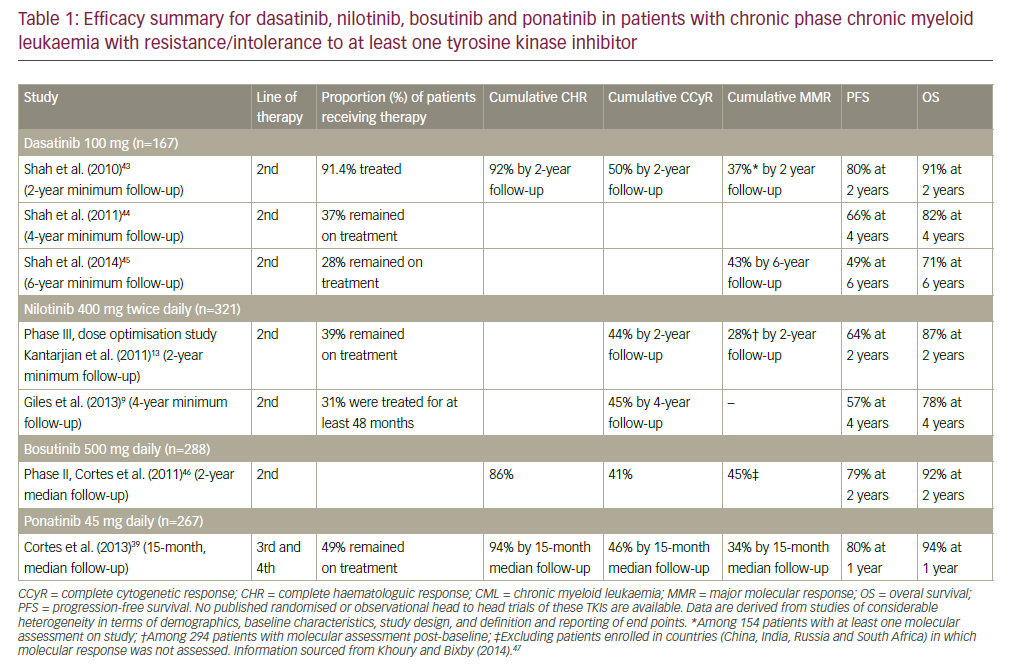
The first IDH1 inhibitor developed on a clinical level is ivosidenib. In the AG120-C-001 phase I study (Study of Orally Administered AG-120 in Subjects With Advanced Hematologic Malignancies With an IDH1 Mutation; ClinicalTrials.gov identifier: NCT02074839), 125 patients with an R/R AML received ivosidenib 500 mg daily.96 Overall response rate (ORR), CR/complete remission with incomplete haematological recovery (CRh) and CR were, respectively, 41.6, 30.4 and 21.6%. The median time to CR was 2.8 months. The overall survival (OS) after a median follow-up of 14.8 months was 8.8 months (Table 1).96–98 The achievement of CR/CRh was significantly associated with a lower co-mutational burden and the absence of mutations in signalling pathways. The D-2HG level has been normalized in almost all cases, consequently being unreliable as a surrogate marker of efficacy.99,100 Thirty-four patients with ND AML who were ineligible for standard induction chemotherapy also received ivosidenib monotherapy. Frontline treatment leads to ORR, CR and CR/CRh of 54.5, 30.3 and 42.4%, respectively. With a median follow-up of 23.5 months, the median OS was 12.6 months with an estimated 1-year OS rate of 51.1%. Again, no single-gene mutation was significantly associated with CR/CRh.101 In the phase III AGILE trial (Study of AG-120 (ivosidenib) vs. placebo in combination with azacitidine in participants with previously untreated acute myeloid leukemia with an IDH1 mutation; ClinicalTrials.gov identifier: NCT03173248), patients with treatment-naive AML unfit for intensive induction chemotherapy were randomly assigned to receive azacitidine and ivosidenib or matched placebo.102–104 The combination therapy with ivosidenib demonstrates a high ORR of 62.5%, including 47.2% of the CR rate, versus 18.9 and 14.9% in the placebo arm (p<0.0001 and p<0.0001), respectively. Responses were seen across cytogenetic risk groups and mutations.105 The combination of ivosidenib and azacitidine had a favourable safety profile with fewer infections (28.2%) relative to the placebo plus azacitidine arm (49.3%). The median OS for responders was 29.3 versus 7.9 months in the placebo arm (p=0.001). The combination is approved by the FDA and European Medicines Agency.
Table 1: Efficacy and safety data of phase I/II trials of ivosidenib and olutasidenib in relapsed/refractory acute myeloid leukaemia96–98
| Study details | ||||
| Author (year) | Di Nardo (2018)96 | Watts, 202397 | De Botton, 202398 | Watts, 202397 |
| Trial name | AG120-C-001 study | 2102-HEM-101 study | 2102-HEM-101 study | 2102-HEM-101 study |
| ClinicalTrials.gov identifier | NCT02074839 | NCT02719574 | NCT02719574 | NCT02719574 |
| Phase | Phase I | Phase I | Phase II | Phase I |
| Treatment | Ivosidenib | Olutasidenib | Olutasidenib | Olutasidenib + AZA |
| Number of patients | 125 | 22 | 147 | 26 |
| Median age, years | 67 | 72 | 71 | 67 |
| Efficacy | ||||
| CR, % | 21.6 | 18 | 32 | 12 |
| Median time to CR, months | 2.8 | 1.9 | 1.9 | 1.9 |
| CR/CRh, % | 30.4 | 32 | 35 | 16 |
| ORR, % | 41.6 | 41 | 48 | 46 |
| Median duration of CR/CRh, months | 8.2 | NA | 25.9 | NA |
| Median DOR, months | 6.5 | NA | 11.7 | NA |
| Median OS, months | 8.8 | 8.7 | 11.6 | 12.1 |
| Safety: grade 3 or more AEs, % | ||||
| QT prolongation | 8.9 | 0 | 1* | 7† |
| DS | 5.4 | 9 | 8 | 7 |
| Anaemia | 19 | 22 | 20 | 20 |
| Thrombocytopaenia | 13.6 | 28 | 16 | 41 |
| Febrile neutropaenia | 24.8 | 22 | 20 | 28 |
| Hepatic enzyme increase | NA | 16 | 3 | 11 |
*Considered as unrelated to treatment.
†Grade 2–3.
AE = adverse event; AZA = 5-azacytidine; CR = complete response; CRh = complete response with partial haematological recovery; DOR = duration of response; DS = differentiation syndrome; NA = not available; ORR = overall response rate; OS = overall survival.
A high-throughput screening led to the discovery of quinolinone derivatives as specific inhibitors of mIDH1.106 Structure-based design and optimization of candidate compounds generated olutasidenib (FT-2102), a brain-penetrant, potent, selective and orally bioavailable inhibitor of IDH1 R132 mutants. Olutasidenib efficiently inhibits D-2HG production in xenograft models, with no activity against wtIDH1. Olutasidenib is an allosteric inhibitor of mIDH1 and binds a hydrophobic pocket near the heterodimer interface and stabilizes the mutant enzyme in its open inactive conformation.107 Olutasidenib has a different structure and binding properties than ivosidenib, and an in vitro study suggested that it could overcome the resistance to ivosidenib due to second-site mutations.108
Efficacy of olutasidenib
The pivotal multicentre, open-label phase I/II trial 2102-HEM-101 (Open-label study of FT-2102 with or without azacitidine or cytarabine in patients with AML or MDS with an IDH1 mutation; ClinicalTrials.gov identifier: NCT02719574) aimed to evaluate olutasidenib as a single agent or in combination with azacitidine in patients with AML and MDS with IDH1 mutations.97 The FDA approved olutasidenib on 1 December 2022 for adult patients with R/R AML with IDH1 mutations due to a high response rate, durability of the response and favourable safety profile.20 No dose-limiting toxicities were observed in the dose-escalation phase, and olutasidenib 150 mg twice daily in continuous 28-day cycles was identified as the recommended phase II dose.109
Response and survival with olutasidenib as a single agent
The phase I study enrolled adult patients with AML and MDS who were R/R or unfit for standard treatment (Table 1). The patients were allocated to receive olutasidenib as a single agent or in combination with azacitidine if they were eligible for hypomethylating agents. Between 2014 and 2016, 32 patients received olutasidenib as monotherapy, including 22 (69%) R/R AML and 4 (15%) with treatment-naive AML. The median age was 72 years. Among patients with R/R AML, CR, CR/CRi and ORR were 18% (95% confidence interval [CI], 5–40), 32% (95% CI, 14–55) and 41% (95% CI, 21–64), respectively. The median time to the first response was 1.9 months. The median OS was 8.7 months (95% CI, 2.5–not estimable [NE]). The estimated 12-month OS was 44% (95% CI, 23–64). Median progression-free survival (PFS) was 16.3 weeks (95% CI, 5.1–24.0). These results are similar to those reported for ivosidenib in a comparable population of patients with AML.99 Among treatment-naive patients, ORR was 25% (one of the four), median OS was 8.8 months (95% CI, 0.6–14.5) and the 12-month OS was 50% (95% CI, 6–85).109
A preplanned interim analysis in patients with mIDH1 R/R AML who received olutasidenib alone in the pivotal phase II cohort of the trial confirmed the encouraging results of the phase I study (Table 1).98 Efficacy was evaluated in 147 patients who received the first dose of olutasidenib at least 6 months before data cut-off. CR, CR/CRh (primary endpoint) and OR were achieved in 32% (95% CI, 24.5–40.2), 35% (95% CI, 27.0–43.0) and 48% (95% CI, 40.0–56.7), respectively. The median duration of response (DOR) was 11.7 months (95% CI, 6.9–25.9), the median duration of CR was 28.1 months (95% CI, 13.8–NE) and the median duration of CR/CRh was 25.9 months (95% CI, 13.5–NE). The median OS was 11.6 months (95% CI, 8.9–15.5) and correlated to response: the median OS was not achieved in patients who reached CR/CRh and was 4 months for non-responders. Responders had lower IDH variant allele frequency (VAF) at diagnosis, fewer co-mutations, less FLT3 mutations and less receptor tyrosine kinase (RTK) pathway mutations. Of note, patients with IDH1 R132H mutation had a relatively lower CR/CRh rate compared with other mutation subtypes and tended to have more co-mutations, particularly mutations in NPM1 and RTK genes, including FLT3.
Response and survival with olutasidenib in combination with azacitidine
Among patients with R/R AML treated in the combination therapy group of the phase I study, ORR was 46% (95% CI, 27–67). Twelve per cent (95% CI, 2–30) of patients achieved CR. The median time to the first response was 1.9 months, and the median DOR was 2.0 months (95% CI, 0.9–3.2). The median OS was 12.1 (95% CI, 4.2–NE) months (Table 1). The estimated 12-month OS was 54% (95% CI, 32–71). The median PFS was 19.6 weeks (95% CI, 11.1–23.7). Among the 13 patients with treatment-naive AML treated in the combination arm, the ORR was 77%. The median DOR and median OS were not reached. The estimated 12-month OS was 75% (95% CI, 41–91).109,110
Haematological improvement
Red blood cell (RBC) and/or platelet transfusion independence (TI) during any 56-day post-baseline period was achieved in patients treated with olutasidenib as a single agent as well as in patients treated with the olutasidenib–azacitidine combination. Forty per cent and 34% of patients under olutasidenib alone achieved TI during the phase I and phase II parts of the trial, respectively. In the combination group of the phase I study, 33% of patients with AML achieved TI. TI was correlated to response, as 100% and 88% of patients achieving CR/CRh in the phase II study reached platelet and RBC TI, respectively. Most patients with an abnormal absolute neutrophil count at baseline had improvement on treatment.98,109,110
Molecular response
In the phase I study, a significant reduction in IDH1 VAF of <1% was observed in 40% of patients with AML who had a response. One patient in the olutasidenib group and one patient in the combination therapy group obtained molecular clearance by NGS.109 In the phase II study, molecular clearance was correlated to response with 28% of VAF clearance in patients with CR/CRh, 8% of VAF clearance in other responders and 7% of VAF clearance in non-responders. After two cycles, the median D-2HG concentration was reduced by 82% in responders.98
Toxicity of olutasidenib
In the 2102-HEM-101 trial, olutasidenib had a favourable safety profile similar to that of ivosidenib (Table 1).98,109,110 All patients reported at least one adverse event (AE) of any grade, irrespective of the relation to olutasidenib. In both phase I and II studies, the most frequent AEs of any grade (mostly grade 1/2) were gastrointestinal disorders (nausea, constipation, diarrhoea and vomiting), pyrexia, fatigue, dyspnoea and hypokalaemia. Among grade 3–4 AEs, haematological AEs were the most frequent. Grade 3–4 thrombocytopaenia, febrile neutropaenia and anaemia occurred in around 20% of patients receiving olutasidenib as a single agent and neutropaenia in around 10% of them. Grade 3–4 thrombocytopaenia and febrile neutropaenia were more frequent in the combination therapy group (41 and 28%, respectively). Of note, other AEs were similar for olutasidenib given as monotherapy or in combination.
Around 75% of patients presented serious AEs, including disease progression, febrile neutropaenia, pneumonia and differentiation syndrome (DS). Thirteen per cent of patients in both arms of the phase I study and 14% of patients in the olutasidenib arm of the phase II study had DS of all grades. Grade 3–4 DS was reported in 9% of patients receiving olutasidenib as a single agent and in 7% of patients in the combination arm, mostly during cycle 1. Most of them were successfully managed with olutasidenib interruption or dose reduction, dexamethasone, hydroxycarbamide and diuretics. The rate of DS with olutasidenib is similar to that reported with ivosidenib.99 Grade 3–4 hepatic AEs of special interest occurred in around 15% treated with olutasidenib alone and in 11% of patients on combination treatment. The most frequent event was an increase in laboratory liver function parameters. None led to the criteria for Hy’s law or liver failure. Fatal AEs were reported in 34% of patients treated in the olutasidenib arm of the phase I study, in 31% of patients treated in the olutasidenib arm of the phase II study and in 20% of patients in the phase I combination therapy. The most common fatal AEs were disease progression (in 9, 14 and 9% of patients, respectively) and infections. QT interval prolongation occurred in 7% of patients of the phase I cohort and 8% in the monotherapy arm of the phase II cohort. None of them was reported as serious, all were transient and no treatment interruption was required. Of note, these patients were frequently taking concomitant medications associated with QT prolongation. In conclusion, AEs were mostly expected and highly manageable with dose modification and standard-of-care measures. The toxicity profile of olutasidenib seems to be quite similar to that of ivosidenib.
Discussion
The discovery of IDH mutations allowed the development of a new class of drugs, mIDH inhibitors. The efficacy of these new molecules in preclinical studies and in clinical trials validated mIDH targeting as an effective treatment strategy.
The tolerance of mIDH inhibitors is excellent. Olutasidenib has a safety profile similar to that of ivosidenib (Table 1). Their side effects are well characterized and easily manageable with dose modifications and standard-of-care measures, allowing their administration to patients unfit for standard therapies, even in the elderly.111 Ivosidenib as a single agent has proven its clinical efficacy in heavily pre-treated or unfit patients with AML with clinical benefits.99,101 Similar response rates are observed with olutasidenib in a similar population of patients treated in the 2102-HEM-101 trial (Table 1). DOR with olutasidenib is promising.98,109 More interesting results are obtained with the combination of mIDH inhibitors with hypomethylating agents.112 In the phase III AGILE trial, a clear clinical benefit was observed in the ivosidenib arm with a significant survival improvement compared with the placebo arm.102 Results of the combination of olutasidenib and azacytidine in the phase I study of the 2102-HEM-101 trial are promising, especially in patients with ND AML, and the data of the phase II part of the trial are eagerly awaited.109
Moreover, the development of new molecules, such as the BCL2 inhibitor venetoclax, allows the administration of a triplet regimen, which appears well tolerated and could potentially overcome resistance to treatment.113 A phase I clinical trial showed the feasibility of the association of ivosidenib with intensive chemotherapy for ND patients with AML with encouraging clinical activity.114 A phase III randomized clinical trial is ongoing to evaluate the benefit of adding IDHm inhibitors to chemotherapy in frontline (A study of ivosidenib or enasidenib in combination with induction therapy and consolidation therapy, followed by maintenance therapy in patients with newly diagnosed acute myeloid leukemia or myedysplastic syndrome EB2, with an IDH1 or IDH2 mutation, respectively, eligible for intensive chemotherapy [HOVON150AML], ClinicalTrials.gov identifier: NCT03839771). Of note, olutasidenib crossed the blood–brain barrier and exerted clinical activity in a phase Ib/II trial of R/R mIDH1 gliomas. It could, therefore, be of interest in patients with AML with central nervous system involvement.
Conclusion
Olutasidenib has encouraging clinical activity in the treatment of unfit patients with R/R or AML allowing clinical improvement, with a safe toxicity profile. Only a direct comparison with ivosidenib could highlight the differences in the efficacy and safety of these drugs. However, DORs to olutasidenib seem particularly promising. The efficacy data of olutasidenib in combination with azacytidine are awaited.