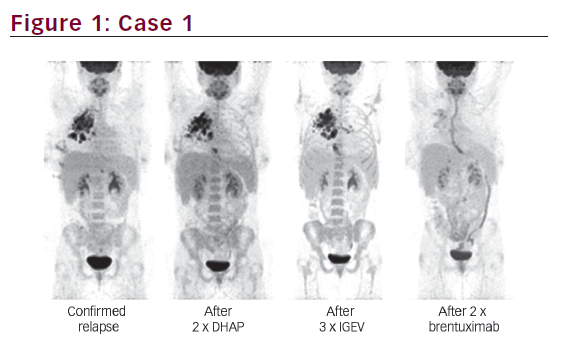
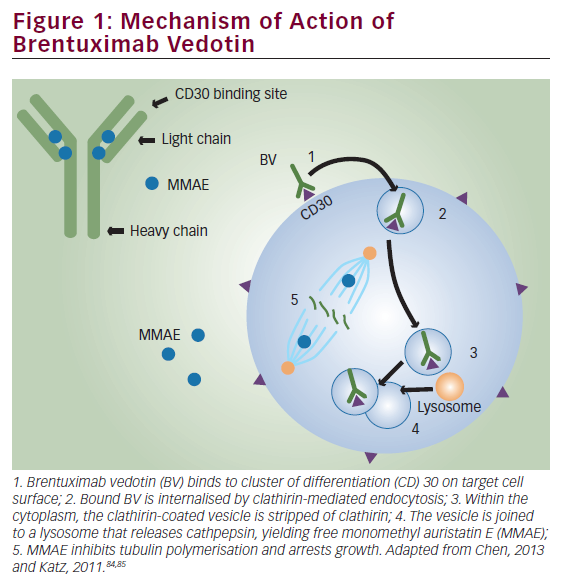
F18-fluorodeoxyglucose positron emission tomography (FDG-PET), commonly combined with computed tomography (CT), is widely used in the initial evaluation and response assessment of patients with Hodgkin’s lymphoma (HL). Its sensitivity for nodal and extranodal sites of disease can add to the staging information obtained with CT alone,1 and PET is valuable in the response assessment at the end of front-line therapy because it can distinguish active disease from fibrosis in residual masses. In fact, the goal of front-line therapy is now a PET-negative complete remission (CR).2 Interim PET scan, performed during the initial course of therapy, may also have prognostic significance,3 and treatment adapted to interim PET results is under investigation in ongoing clinical trials.
The role of PET in the response assessment and management of relapsed and refractory HL is less well established than in the front-line setting. Up to 30 % of patients with HL will fail to respond to, or will relapse after, initial therapy, and approximately 50 % of these patients can achieve durable disease-free survival with salvage chemotherapy and autologous stem cell transplant (ASCT). Retrospective studies have consistently demonstrated the prognostic significance of a PET scan performed prior to ASCT, although it is unclear how those PET results should guide the choice of salvage therapy or the transplant approach. This article will focus on the role of PET in the management of patients with relapsed or refractory HL who are candidates for ASCT. It will also address the limited evidence for the use of PET in relapsed HL patients who are not undergoing ASCT.
Positron Emission Tomography in Patients Undergoing Autologous Stem Cell Transplant
Prognostic Significance of Pre-transplant Positron Emission Tomography
Over the past two decades, several groups have identified clinical factors that predict the outcome of salvage therapy in patients with relapsed or refractory HL.4–9 They identified adverse factors that include time to relapse less than one year, advanced stage or extranodal disease at relapse, and various components of the International Prognostic Score,10 such as hypoalbuminemia, anemia, older age, and lymphopenia. Because the various proposed prognostic scores are based on factors present at the time of relapse, without incorporating subsequent information about response to salvage therapy, they have the potential to influence the choice of salvage chemotherapy. However, in practice, most patients with relapsed or refractory HL are candidates for ASCT and are treated with standard aggressive combination chemotherapy, regardless of their relapse prognostic score. Instead of clinical factors at relapse, the response to the salvage chemotherapy has emerged as the most important predictor of progression-free survival (PFS) and overall survival (OS) in relapsed HL, and that response is most accurately determined by PET.
To view the full article in PDF or eBook formats, please click on the icons above.