Nonetheless, radiologists are frequently asked by clinicians to identify which patients MRI should be used for as the first choice to help accurately establish the clinical staging of HNSCCA. There is no easy answer to this question as the head and neck regions comprise a variety of different anatomical sites and each imaging method has its merits. Both MRI and CT can provide acceptable results, and which mode of imaging should be used is controversial. The practical choice may depend on factors such as local availability, scanning time and cost. However, if MRI is available and no contraindications appear (see Table 1), the procedure could be recommended as a primary imaging technique for the patients who will benefit from MRI. See below for a discussion on separate entity stagings according to T, nodal (N) and metastatic (M).
Tumour Staging
According to the sixth edition of American Joint Committee on Cancer (AJCC) Cancer Staging Manual,1 cross-sectional imaging in the nasal cavity, paranasal sinus and nasopharyngeal carcinomas is mandatory to complete the staging process. MRI is the preferred method and the given alternative is CT with contrast. For oral cavity, oropharyngeal, hypopharyngeal and laryngeal carcinomas, the assessment of the primary tumour is based primarily on clinical examination and crosssectional imagings (CT or MRI) is recommended to be used when the deep tissue extent of the primary tumour is in question.
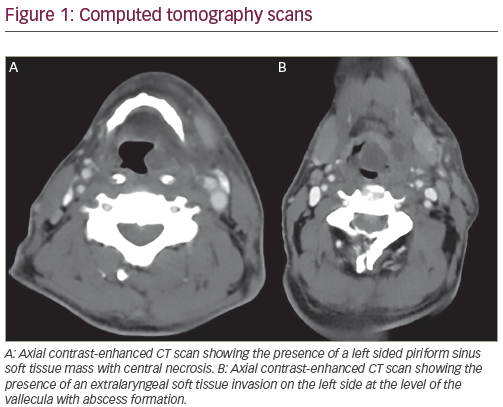
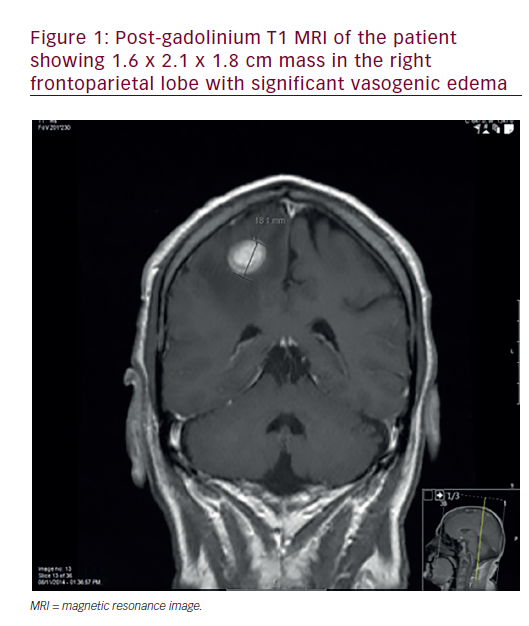
MRI is the best method for delineating the extent of the intraorbital, intracranial extension and peri-neural spreading, which are commonly detected in carcinomas of the nasal cavity, paranasal sinus and nasopharynx. The presence of intracranial dural infiltration, best detected by MRI, will also upstage the nasal cavity and paranasal sinus carcinomas to be an unresectable tumour stage T4b. Although the linear enhancement of dura does not always imply dural infiltration by a tumour – and it can frequently be difficult to differentiate from benign reactive change, the presence of pial enhancement – focal dural nodules or dural thickening of more than 5mm is highly accurate when predicting the presence of neoplastic dural invasion.2 In nasopharyngeal carcinoma, MRI has been reported to change almost 40% of tumour stages compared with CT in the recent study by Sun et al.3 MRI can also easily differentiate any head and neck cancers that invade paranasal sinus from benign inflammatory mucosal thickening or retained secretion, all of which give similar findings and cannot be easily differentiated by CT (see Figure 1). However, high-resolution CT may be used as an additional complementary examination to provide a better and easier demonstration of thin cortical bony erosion in nasal cavity and paranasal sinus carcinomas. Some radiologists have also shown a distinct preference for the CT scan detail in nasopharyngeal carcinoma of the cortical skull base erosion.4
When the deep tissue extent of the primary tumour in an oral cavity and oropharyngeal carcinoma is still in question, MRI may be recommended as the best method of diagnosis.5,6 Apart from tumour size, which can be measured by either CT or MRI, invasion of the deep extrinsic tongue muscles is another important part of tumour staging and tumours of any size will be upstaged to T4a whenever this phenomenon is observed (see Figure 2). Various tongue movements by a patient, commonly used to assess the presence of deep extrinsic tongue muscle invasion during a clinical examination, are not precise enough to determine definite tumour invasion. A high prevalence of misdiagnosis for base of tongue carcinomas (a subsite of the oropharynx) by clinical examination alone has been reported to be as high as 50% in T2, 85.7% in T3 and 16.7% in T1, but not a single misstaging was found in T4a and T4b.7 Perhaps MRI should be recommended as mandatory for all patients with oral or oropharyngeal carcinomas whose clinical examinations suggest stage T2 or T3 tumours to be certain that the tumour stages are not already at T4 before treatment begins.
Since most changes were due to finding invasion of the deep extrinsic tongue muscles that could be detected only from imaging, while the currently accepted clinical staging criteria were established based mainly on clinical examinations, should we reconsider how the ‘imaging up-staging’ may affect the prognosis, especially considering the slight invasions of the deep extrinsic tongue muscle criteria? Perhaps the AJCC staging system should be revised to allow for ‘minor’ involvement of extrinsic tongue muscles seen only by imaging but that are not to be upstaged to T4a. Alternatively, the guidelines could be revised to reflect more practically used terms such as ‘tongue fixation or limited tongue movement in various fashions by clinical examination’ instead of ‘deep extrinsic tongue muscle invasion’.
Although the maximum diameter of a tumour in oral cavity and oropharynx has mainly been used in the T staging system, tumour thickness is also a significant independent prognostic factor in predicting subclinical nodal metastasis, local recurrence and patient survival in oral tongue carcinoma,8,9 but this can only be accurately measured by MRI.10 Research has shown that a tumour 3mm thick or smaller has 8% subclinical nodal metastasis, 0% local recurrence and 100% five-year actuarial disease-free survival; a tumour 3–9mm thick has a 44% subclinical nodal metastasis, 7% local recurrence and 76% five-year actuarial disease-free survival; and a tumour 9mm or more thick has 53% subclinical nodal metastasis, 24% local recurrence and 66% fiveyear actuarial disease-free survival.9 Therefore, pre-operative assessment of tumour thickness by MRI is invaluable in planning treatment of an oral tongue carcinoma.
Mandibular invasion is another poor prognostic sign in oral cavity and oropharyngeal carcinoma. MRI has been proved to provide high sensitivity, specificity and accuracy (93%) with a high negative– predictive value of up to 96% in demonstrating mandibular invasion.6 This may suggest that MRI is a reliable technique for ruling out neoplastic invasion of the mandible. In addition, MRI has an excellent diagnostic value for both cortical erosion and neoplastic replacement of medullary bone that allows appropriate selection of surgical strategy i.e. marginal mandibulectomy for cortical invasion or segmental mandibulectomy for medullary bone invasion. Although high-resolution CT can provide high sensitivity and specificity when mandibular invasion is assessed, especially cortical bone invasion,11–13 commonly seen beamhardening artefacts produced by dental amalgam or prosthetic implants can spoil the quality of images and limit correct assessment of the problem. Susceptible artefacts from dental work generally obscure the underlying anatomy less on MRI than artefacts created by CT. However, a number of false-positive cases of mandibular invasion diagnosed by MRI have been found and may be caused by other disease processes such as inflammatory odontogenic disease, post-extraction bone defect, osteoradionecrosis or normal variation of the cortex. Furthermore, chemical shift artefacts produced by the mandible’s bone marrow may obscure the black line of the mandibular cortex and mimic cortical invasion,12 in which case high-resolution CT may be used as an additional complementary examination in these vague cases to confirm or exclude the cortical invasion.
Not all laryngeal and hypopharyngeal carcinomas require imaging. T1 glottic carcinoma and small or superficial tumours can be accurately staged by clinical examination. In these cases, cross-sectional imaging is unnecessary unless deeper invasion is still suspected.14 Significant underestimated tumour stagings in larger tumours have been found, and combined imaging with clinical examination is recommended whenever a clinical examination suggests other tumour stages (T2 or above). Valuable information can also be more accurately provided through MRI for accurate tumour staging when related to the deeper tumour extensions such as invasion of the base of the tongue, pre-epiglottic and paraglottic spaces or cartilage invasions.
In spite of many recent technical improvements, a standard MRI examination of both the larynx and hypopharynx still takes a relatively longer time and requires more co-operation from the patient than a standard helical CT examination. Dyspnoea predisposes to motion artefacts and is a frequent problem found in patients undergoing imaging studies of the larynx and hypopharynx. Therefore, we prefer CT as the primary imaging in patients with laryngeal or hypopharyngeal carcinomas. MRI is preserved for cartilage assessment in a candidate for partial laryngectomy to make sure that there is no cartilage invasion, since MRI has been shown to be more sensitive and slightly more accurate than CT in identified cartilage involvement.15,16
Invasion of the pre-vertebral space will upstage laryngeal and hypopharyngeal carcinomas, thus giving a poor prognosis and unresectable tumour stage T4b. Preservation of the high-signalintensity fat strip that lies between the tumour and the prevertebral musculature on the unenhanced T1-weighted images can reliably predict the absence of prevertebral space fixation.17 However, MRI is rather poor in predicting involvement of the prevertebral space and may not be able to differentiate between neoplastic fixation and nonneoplastic changes in the pre-vertebral space. An abnormal muscle contour, T2 hyperintensity and enhancement are present not only in neck carcinomas that are fixed to the pre-vertebral space but also in patients in whom the tumour is mobile and resectable.18 Open neck exploration with direct evaluation of the pre-vertebral muscles is superior to both CT and MRI and it should continue to be the standard of care unless there is an intact high-signal-intensity fat strip detected on T1-weighted images.18,19
Timing is crucial in imaging a primary tumour. In order to get an accurate measurement of any primary tumour, MRI should be performed prior to surgical biopsy. Nevertheless, many patients have come to imaging after having had a recent biopsy. This may subsequently produce an abnormal signal due to haemorrhage and oedema, and consequent misinterpretation as a tumour. A suggestion has been made for a delay of between 10 and 14 days post-biopsy to overcome this problem.20 However, the timing is controversial and is also influenced by the clinical management in each hospital. It is important to realise that mucosal lesions are better assessed by clinical examination, while the deeper submucosal extensions are better assessed by cross-sectional imagings. Some small superficial mucosal tumours may go undetected by MRI, and both clinical examination and MRI should therefore contribute equally important information for the staging assessments.
Nodal Staging
If either a CT or MRI is undertaken for the purpose of primary tumour evaluation, simultaneous imaging assessment of the nodal involvement should be performed since the presence of a cervical metastatic node is a major determinant in the patient’s prognosis of head and neck cancer. For all head and neck sites, the presence of a solitary ipsilateral or contralateral positive lymph node or extracapsular tumour spread will reduce the expected survival of a patient by nearly 50%.21 The incidence of nodal disease in HNSCCA depends on the primary tumour site and varies between less than 10% in glottic carcinoma to about 65, 75 and 85% in hypopharyngeal, oropharynx and nasopharyngeal carcinomas, respectively.22 As MRI has no advantage over CT for the examination of cervical lymphadenopathy,3,23 it may not be necessary for nodal staging. Consequently, CT may be a good choice for this purpose because it requires much less time for image acquisition for a whole neck examination and it can also show extracapsular tumour spread of lymph nodes sooner than MRI.13 Nevertheless, MRI is better than CT in detecting retropharyngeal lymph nodes and in distinguishing the lymph node from the adjacent primary tumour.
It is interesting to note here the significance of retropharyngeal lymphadenopathy in affecting clinical staging for the different primary sites of HNSCCA. Enlargement of the retropharyngeal lymph nodes can be detected only from cross-sectional imaging and not by clinical examination. Nasopharyngeal carcinoma is the most common primary malignancy that spreads to retropharyngeal lymph nodes. However, the retropharyngeal lymph node is of no prognostic significance in nasopharyngeal carcinoma. The presence or absence of retropharyngeal lymph node metastasis does not affect the prognosis of the patient and is currently still not included in the TNM staging system of nasopharyngeal carcinoma.4 However, retropharyngeal lymphadenopathy arising from other primary lesions such as oropharyngeal or hypopharyngeal carcinomas indicates a worse prognosis and should be considered as cervical lymph nodes for staging purposes.24 If left unrecognised, these lymph nodes will not be included in the standard neck dissection and may also be underdosed in standard radiation ports for oropharyngeal or hypopharyngeal carcinomas.
The lack of specificity remains the most commonly used size criteria in the diagnosis of metastatic nodes using both CT and MRI. The recent introduction of functional MRI using an iron-contrast-agent-enhanced MRI (dextran-coated superparamagnetic iron oxide particles [SPIO]) of the head and neck has been reported to provide a high sensitivity of 86% and specificity of 100% in identified metastatic nodes.25 However, this contrast agent is still not as widely used, due not only to the relatively expensive price but also to the cumbersome procedures to use this contrast agent on a routine basis. The administration of this contrast agent takes about 30 minutes and MRI is needed both before and after administration of SPIO so the patients have to come back to the department twice and undergo two separate studies, which doubles the cost of examination. Further development of this contrast agent for more convenient use is needed before it will gain more widespread acceptance. Distant Metastases
Exclusion of distant metastases is important in staging and prognosis of HNSCCA. Currently, MRI still has a limited role in searching for the presence or absence of distant metastases. Most of these tasks are performed by other imaging methods and the protocol may vary between institutions. Various imaging procedures such as chest X-ray, ultrasound, CT, MRI and isotope bone scan may be needed in the more advanced local or nodal disease. This approach is time-consuming and can still miss lesions outside the fields of study.
Although becoming increasingly popular in the metastatic work-up, the role of whole-body technologies to offer a complete head-to-toe coverage of the patients in a single examination such as positron emission tomography–computed tomography (PET-CT) is limited. Apart from the high cost of examination, another disadvantage of PET-CT is the considerable amount of applied ionising radiation: approximately 25mSv through the radioactive tracer and diagnostic spiral CT.26
The recently introduced multichannel MR scanners with automated free table movement and the use of acquisition acceleration techniques have made whole-body MRI (WB-MRI) clinically feasible providing a high image quality within a reasonable examination time (less than one hour). WB-MRI is highly sensitive in detecting distant metastases, has shown its superiority particularly in the detection of liver, bone and brain metastases and has a higher overall diagnostic accuracy in the detection of distant metastases of 92% compared with only 82% for PET-CT because of its excellent contrast in soft tissue and parenchymal structure.27 Herborn et al.28 have also reported 100% accuracy in determining the overall TNM category in patients with advanced HNSCCA using WB-MRI compared with the standard of reference (chest X-ray, ultrasonography, CT of head, neck and thorax, endoscopy and histology).
Cancer is characterised not only by pathological metabolism (e.g. highglucose uptake detected by PET) but also by a higher cellularity. A malignant tumour often has a larger cell diameter and denser cellularity than normal tissue, which results in restriction of water diffusion.
Therefore, diffusion-weighted imaging (DWI) has recently been applied for imaging metastasis by Takahara et al.29 Their initial results have demonstrated that DWI in WB-MRI is a feasible clinical technique in improving the assessment of metastatic spreading. Furthermore, another study found a high concordance between DWI and PET-CT scans, with the ‘PET-like’ WB-MR images also being impressively produced in the detection of distant metastases by inversion of the original DWI images in WB-MRI.30
The increasing number of new MRI systems installed in most parts of the world and their lower cost compared with PET-CT examinations should further ensure the benefit of WB-MRI application in oncology by offering new options for systemic secondary tumour screening, making it possible to reduce the number of necessary separate radiological examinations and thus time in oncologic staging.
Conclusion
Although controversial, MRI should be recommended as the first choice in tumour staging for nasal cavity, paranasal sinus, oral cavity, oropharyngeal and nasopharyngeal carcinomas, with CT as an alternative. CT may be the primary imaging method in hypopharyngeal and laryngeal carcinomas, with MRI reserved for cartilage invasion assessment in a candidate for partial laryngectomy.
With the development of WB-MRI techniques to assess distant metastases, it may be possible, in the near future, to see the role of MRI as a ‘one-stop shop’ modality in accurately establishing the clinical staging of HNSCCA.