Malignant pleural mesolthelioma (MPM) is a locally aggressive cancer that arises from the multipotential mesothelial cells of the pleura. MPM has a uniformly poor prognosis with a median survival from diagnosis of nine to 12 months.4 Limited treatment options are available for those diagnosed with MPM or at risk for developing MPM from past or ongoing asbestos exposure. While rare, MPM is responsible for approximately 0.6% of all cancer-related deaths.5 MPM poses an increasing public health, medical, and economic problem. This is due to the peak commercial use of asbestos in industrialized countries between the 1930s and the 1960s and the latency in developing MPM from the time of first exposure, which ranges from 15 to 40 years.6,7 In addition, asbestos continues to pose a public health hazard throughout the world due to the need for its disposal and its current and increasing use in industrializing nations. Recent estimates report an expected incidence of 2,000–3,000 cases per year in the US, 1,950–2,450 cases per year in the UK, and 250,000 deaths caused by MPM in Western Europe over the next few decades.1,8,9
In addition to the direct costs to the healthcare system, defendant companies in the US have already paid $54 billion in legal claims and are expected to face upwards of $200 billion in future liabilities, thus representing a significant socioeconomic burden.5 Interestingly, only 5% of asbestos mine workers who have experienced heavy exposure to asbestos go on to develop MPM, a fact that illustrates the complex relationship between environment, biology, and genetics in MPM.10 In addition, the characteristically long latency time for developing MPM suggests that the multiple somatic abnormalities common in MPM accumulate within the mesothelial cells over time and contribute substantially to the pathogenesis of MPM. Recent research has implicated multiple molecular pathways and genetic loci that are abnormal in MPM, and has increased our understanding of the pathogenesis of the disease. These insights may provide possible therapeutic targets for treatment and prevention.
Pathogenesis
The mechanism of asbestos-induced MPM is unclear. Genomic and molecular analyses have elucidated multiple cytogenetic and molecular abnormalities that contribute to the development of MPM. It is commonly believed that asbestos inhalation leads to the deposition of fibres deep in the lung parenchyma and eventual migration and implantation of fibers into the pleural lining. Repeated episodes of inflammation and healing, oxygen free radical production from inflammatory cells and the iron moiety within asbestos,11–13 and direct damage to DNA by the fibers are generally accepted pathogenic features of asbestos exposure.4 Interestingly, dose-dependent cytotoxicity of asbestos is not lethal to the asbestos-sensitive mesothelial cells.14,15 The inflammatory response to asbestos deposition in the pleura is mediated by macrophages and mesothelial cells, with both cell types secreting tumor necrosis factor (TNF)-α and the mesothelial cell expressing TNF-α receptor (TNF-R1) in an autocrine and paracrine interaction. TNF-α then stimulates the nuclear factor kappa B (NF-κB) pathway, which regulates pro-survival cellular mechanisms and may allow asbestos-induced DNA-damaged cells to divide rather than undergo apoptosis.
This response imparts a survival advantage that permits the asbestos-injured cells to transform and progress into malignant mesothelioma.16 Based on these findings, high-risk cohorts in Turkey will be treated with ranpirnase, a ribonuclease (RNase) that inhibits NF-κB activation, which will hopefully block this pathway and help prevent the development of MPM. Considerable controversy regarding the role of simian virus 40 (SV40) in the pathogenesis of MPM persists today. SV40 is a rhesus monkey DNA virus, likely introduced to humans from contaminated Salk polio vaccines produced between 1955 and 1978.17 SV40 has been associated with the development of MPM in humans and animal models.18,19 Overall, the role of SV40 in MPM is a controversial topic.
Presentation
A person with MPM will usually be male and between 50 and 70 years of age, and will report a significant history of asbestos exposure. The most common symptoms upon presentation include dyspnea and chest pain. More than 50–70% of patients report dyspnea and 60% present with non-pleuritic chest pain that is typically located in the posterolateral thorax. Physical findings are directly related to the extent and natural progression of disease. Eighty percent of patients will present with a pleural effusion and dyspnea, and 95% will develop an effusion at some point during the course of their disease.10 Extension of the tumor through the diaphragm can result in malignant ascites.
Laboratory Analysis and Serum Markers
Laboratory findings are generally non-specific and can include hypergammaglobulinemia, an elevated erythrocyte sedimentation rate (ESR), anemia, and, most strikingly, thrombocytosis (>400,000), which is seen in upwards of 30–40% of patients. Recent research has identified serum mesothelin-related protein (SMRP) and osteopontin as promising new serum markers for identifying and following patients with MPM. A Mesothelin enzyme-linked immunosorbent assay (ELISA) (MesoMark™) is currently available for clinical use in Europe and Australia and through reference laboratories in the US.
Imaging
Computed tomography (CT) of the chest remains the most useful imaging study in MPM. CT can identify pleural changes associated with asbestos exposure and MPM such as pleural thickening, calcified plaques, and pleural effusions, localized nodular mass with pleural effusion, and intrapulmonary nodules in 60% of cases, but is not sensitive in diagnosing chest wall or diaphragmatic involvement.20 MRI has recently been proved to be more sensitive in diagnosing chest wall invasion and diaphragmatic invasion.21
Positron emission tomography (PET) has been used at multiple centers in the US, and early data suggest PET is helpful in identifying benign and malignant pleural disease (MPM in particular) in individuals exposed to asbestos.22 PET may be useful in determining the extent of distant metastatic disease, but had a sensitivity of only 11% in detecting metastatic lymph node disease.23
Diagnostic Approach
Since pleural effusion is such a common presenting sign in MPM, thoracentesis is routinely the first diagnostic procedure attempted and succeeds in diagnosing approximately 30–50% of cases.24 Video-assisted thoracoscopy (VATS) is useful when thoracentesis results are negative, can provide a diagnosis in 80% of patients, and provides excellent visualization of the extent of disease.25 When tumor volume precludes thoracoscopy, open biopsy should be performed in an intercostal space that can later be excised with a more definitive operation. There are three main histological subtypes of MPM: eithelial tumors account for 50–60% of MPMs and carry a better prognosis; sarcomatoid MPMs account for 10% of cases and are the most resistant to therapy, with a mean survival less than one year; and mixed (or biphasic) tumors account for 35% of MPMs. MPM is generally positive for cytokeratin, calretinin, and WT1 and negative for CEA, CD15, TTF-1, and B72.3 It is generally accepted that positive staining for cytokeratin and calretinin with negative staining for three epithelial markers is sufficient to make the diagnosis of MPM. In difficult diagnostic circumstances, electron microscopy usually makes the definitive diagnosis.
Staging
Historically, staging for MPM used non-standardized criteria that resulted in substantial differences in the reported rates of survival and treatment efficacy. In response, the International Mesothelioma Interest Group (IMIG) published their guidelines for the staging of MPM that more accurately documented the progression of disease and the importance of nodal involvement.26 The American Joint Commission on Cancer (AJCC) has adopted these guidelines, and the current tumor, node, metastasis (TNM) staging system used is generally accepted. Staging is essential for operative planning. Patients with stage I–III disease are candidates for surgical cytoreduction. In an effort to stratify patients for survival, Cancer and Leukemia Group B (CALGB) and European Organization for Research and Treatment of Cancer (EORTC) studies found that performance status is the best predictor of survival, while age, histological subtype, and gender are other important prognostic factors.27,28
Treatment Modalities
To date, there are no generally accepted or published treatment guidelines for MPM.29 Recently, the standard treatment regimen for unresectable MPM has been cisplatin plus pemetrexed. This followed a well-powered phase III trial demonstrating longer median survival time and longer time to progression with combined therapy versus cisplatin alone.30 For these patients, control of pleural effusions can be accomplished by thoracoscopic or chest tube pleurodesis with 90% efficacy. PleureX® catheters can be used for poor surgical candidates or recurrent effusions. The main goals of treatment are to control local disease, treat symptoms, and prevent progression and metastasis. Surgery, radiation, chemotherapy, and immunotherapy (generally in combination) have become the common treatment strategies.
Surgery
The common operations used to treat MPM include thoracoscopy for diagnosis or symptomatic control, and extrapleural pneumonectomy (EPP) or pleurectomy/decortication (PD) for curative intent and cytoreduction for adjuvant therapy. Significant debate exists as to whether EPP or PD offers any survival advantage over each other or other treatments. No randomized, controlled trials comparing EPP versus PD or surgery versus non-surgical treatments have been performed, but recent data from Flores et al. point to the efficacy of PD in early-stage mesothelioma compared with EPP.31 The Mesothelioma and Radical Surgery Trial (MARS) trial in the UK, which randomizes patients after chemotherapy to either EPP with radiation or non-surgical therapy, currently aims to determine whether EPP offers any survival advantage. EPP is an en bloc resection of pleura, underlying lung parenchyma, ipsilateral hemidiaphragm, and pericardium. PD attempts to remove all pleural disease without underlying lung and may also include the ipsilateral hemidiaphragm and pericardium in the resection.
Radiation
Thoracic radiotherapy for MPM is limited mainly by the radiosensitvity of the surrounding vital structures of the chest and by the volume of tumor. Curative doses(greater than 60Gy) pose a serious risk to normal tissues including the neighboring lung, heart, esophagus, and spinal cord. Several studies have shown that definitive radiotherapy does not increase median survival past 10 months.32–35 However, Boutin et al. demonstrated that radiotherapy was an effective prophylactic treatment after thoracoscopy to prevent port-site seeding.36
Chemotherapy
Historically, anthracyclines, platinum agents, and antimetabolites have been used as single agents against MPM with poor response rates—ranging from 30 to 40%—and median survival times of less than one year. Combination chemotherapies have had marginally better response rates and median survival times. Platinum-based regimens demonstrated the best response and survival results.37 Symptomatic relief was seen in 40–50% of patients treated with a combination of mitomycin C, vinblastine, and cisplatin.38 Recently, studies using the antimitotic vinca alkaloid vinorelbine as a single agent have shown similar benefit.39 Pemetrexed is a novel antifolate that showed extensive antitumor activity in phase I and II trials.40 A phase III trial enrolled and randomized 456 patients to receive either cisplatin or cisplatin in combination with pemetrexed. The combined regimen proved superior with a three-month longer average survival time and almost a two-month increase in disease-free interval (both statistically significant).30 In addition, the same study noted that vitamin B12 and folate supplementation provided better tolerance and a decreased side effect profile, and thus gave a better response rate. While no drugs have demonstrated efficacy in the relapsed setting, milataxel, a novel taxane analog that can be administered orally, is being studied in a phase II open-label trial in patients with refractory mesothelioma to the pemetrexed cisplatin combination.
Multimodality Therapy
The most promising survival data have been generated in studies that combined surgery with radiation or chemotherapy, or all three modalities.41 Multiple studies in selected patients have confirmed that durable survival could be achieved in early-stage patients without nodal disease, and that EPP could be performed with acceptable operative mortality.42 One benefit of EPP is that post-operative radiation therapy can be given without concern for ipsilateral pulmonary toxicity.43 In a phase II trial of EPP followed by radiation therapy completed at Memorial Sloan-Kettering Cancer Center, Rusch and colleagues demonstrated that some patients could have a durable survival— 27% at three years—and a decreased local recurrence of only 13%.44 In an effort to boost the amount of radiation delivered to the post-operative field, researchers have utilized intensity-modulated radiation therapy (IMRT).45 Intraplueral chemotherapy at the time of surgery is an intriguing method of treatment that has yet to show any improvement in local control or survival rates.
Recently, several studies have reported encouraging results using induction chemotherapy. Weder et al. showed in a small pilot study that neoadjuvant chemotherapy with cisplatin and gemcitabine followed by EPP and post-operative radiation could produce a median survival of 23 months. One- and two-year survival rates were 79 and 37%, respectively.46 In another small study, Flores et al. found that early-stage MPM patients successfully completing a course of neoadjuvant chemotherapy with cisplatin and gemcitabine followed by EPP and 54Gy of radiotherapy had a median survival of 33.5 months.47 A more recent Swiss multicenter phase II trial of induction therapy followed by EPP and radiation that included 61 patients reported the same 23-month median survival in patients who underwent EPP. These data suggest that induction therapy may prolong survival compared with upfront surgery. Post-operative morbidity was 62% and mortality was 3.2%, which is similar to the Brigham experience.48
A multicenter US trial of neoadjuvant pemetrexed and cisplatin (PC) followed by EPP and hemithoracic radiation for resectable MPM that included 77 patients illustrated that trimodality therapy was feasible and that chemotherapy could be successfully delivered to patients in a neoadjuvant setting. However, preliminary median survival was only 16.6 months, below the median survival reported in the aforementioned single-institution studies. However, these results could be explained by the high censorship rates experienced early in this study.49
Targeted Therapies
Epidermal growth factor receptor (EGFR), vascular endothelial growth factor (VEGF), and platelet-derived growth factor (PDGF) are important growth factors involved in MPM pathogenesis that are currently being treated with targeted therapy in several studies. Unfortunately, trials with the EGFR tyrosine kinase inhibitors erlotinib and gefitinib have shown no efficacy.50,51 In addition, imatinib mesylate, an inhibitor of tyrosine kinase activity, has had similar treatment failure.52 Recently, a multicenter, double-blind, randomized, placebo-controlled phase II trial that included gemcitabine and cisplatin with either bevacizumab (Avastin), an anti-VEGF receptor monoclonal antibody, or placebo concluded that the addition of bevacizumab did not affect progression-free survival or median overall survival.53 Other studies with antiangiogenic therapies including thalidomide and PTK787 have had no clinical benefit.54,55 Bortezomib, a proteasome inhibitor, is currently being tested in a multinational, multicenter, phase II study and has shown activity against MPM in pre-clinical studies.56 Furthermore, in phase I trials of oral and IV formulations of vorinostat, suberoylanilide hydroxamic acid (SAHA), a novel histone deacetylase inhibitor, two patients had partial response, prompting a placebo-controlled, randomized phase III study of oral SAHA in relapsed mesothelioma patients.57
Expert Opinion/Five-year Review
MPM continues to impart a dismal prognosis to those diagnosed with the disease. Currently, no standard therapy or consensus exists regarding treatment. The number of MPM cases will likely rise over the next two decades and clinicians specializing in thoracic malignancies will increasingly be called upon to treat these patients. For non-surgical candidates, cisplatin plus pemetrexed is now considered to be the standard of care. Based on the previous success of radical surgery and adjuvant chemoradiation, current trimodality therapy has focused on induction therapy followed by surgery and radiation. The encouraging results of this treatment strategy warrant larger confirmatory trials. The utilization of newer technologies such as PET and gene expression microarray may enable better staging and risk stratification of patients, and thus appropriately directed therapies. Basic science and translational research have led to substantial advances in understanding MPM pathogenesis and molecular mechanisms. The use of proteomics and serum analysis may lead to earlier diagnosis of MPM, earlier treatment, and thus better survival. ■
Malignant Pleural Mesothelioma—A Current Review
Article
References
- Ismail-Khan R, Robinson LA, Williams CC Jr., et al., Malignant pleural mesothelioma: a comprehensive review, Cancer Control, 2006;13(4):255–63.
- Kazan-Allen L, Asbestos and mesothelioma: worldwide trends, Lung Cancer, 2005;49(Suppl. 1):S3–8.
- Tsiouris A,Walesby RK, Malignant pleural mesothelioma: current concepts in treatment, Nat Clin Pract Oncol, 2007;4(6):344–52.
- Robinson BW, Musk AW, Lake RA, Malignant mesothelioma, Lancet, 2005;366(9483):397–408.
- Carbone M, Albelda SM, Broaddus VC, et al., Eighth International Mesothelioma Interest Group, Oncogene, 2007;26(49):6959–67.
- Mossman BT, Kamp DW,Weitzman SA, Mechanisms of carcinogenesis and clinical features of asbestos-associated cancers, Cancer Invest, 1996;14(5):466–80.
- Sluis-Cremer GK, Asbestos disease at low exposures after long residence times, Ann N Y Acad Sci, 1991;643:182–93.
- Hodgson JT, McElvenny DM, Darnton AJ, et al., The expected burden of mesothelioma mortality in Great Britain from 2002 to 2050, Br J Cancer, 2005;92(3):587–93.
- Peto J, Decarli A, La Vecchia C, et al., The European mesothelioma epidemic, Br J Cancer, 1999;79(3-4):666–72.
- Pass HI, Hahn S, Carbone M, Malignant Mesothelioma. In: DeVita, Hellman, Rosenberg (eds), Mesothelioma in Cancer: Principles and Practice of Oncology, Seventh Edition, Philadelphia: Lippincott, 2007.
- Kamp DW, Israbian VA, Preusen SE, et al., Asbestos causes DNA strand breaks in cultured pulmonary epithelial cells: role of iron-catalyzed free radicals, Am J Physiol, 1995;268(3.1):L471–80.
- Shukla A, Gulumian M, Hei TK, et al., Multiple roles of oxidants in the pathogenesis of asbestos-induced diseases, Free Radic Biol Med, 2003;34(9):1117–29.
- Xu A, Zhou H, Yu DZ, Hei TK, Mechanisms of the genotoxicity of crocidolite asbestos in mammalian cells: implication from mutation patterns induced by reactive oxygen species, Environ Health Perspect, 2002;110(10):1003–8.
- Bocchetta M, Di Resta I, Powers A, et al., Human mesothelial cells are unusually susceptible to simian virus 40-mediated transformation and asbestos cocarcinogenicity, Proc Natl Acad Sci U S A, 2000;97(18):10214–19.
- Lechner JF, Tokiwa T, LaVeck M, et al., Asbestos-associated chromosomal changes in human mesothelial cells, Proc Natl Acad Sci U S A, 1985;82(11):3884–8.
- Choe N, Tanaka S, Xia W, et al., Pleural macrophage recruitment and activation in asbestos-induced pleural injury, Environ Health Perspect, 1997;105(Suppl. 5):1257–60.
- Cutrone R, Lednicky J, Dunn G, et al., Some oral poliovirus vaccines were contaminated with infectious SV40 after 1961, Cancer Res, 2005;65(22):10273–9.
- Carbone M, Kratzke RA, Testa JR, The pathogenesis of mesothelioma, Semin Oncol, 2002;29(1):2–17.
- Gazdar AF, Butel JS, Carbone M, SV40 and human tumours: myth, association or causality?, Nat Rev Cancer, 2002;2(12):957–64.
- Rusch VW, Godwin JD, Shuman WP, The role of computed tomography scanning in the initial assessment and the follow-up of malignant pleural mesothelioma, J Thorac Cardiovasc Surg, 1988;96(1):171–7.
- Patz EF Jr, Shaffer K, Piwnica-Worms DR, et al., Malignant pleural mesothelioma: value of CT and MR imaging in predicting resectability, AJR Am J Roentgenol, 1992;159(5):961–6.
- Benard F, Sterman D, Smith RJ, et al., Metabolic imaging of malignant pleural mesothelioma with fluorodeoxyglucose positron emission tomography, Chest, 1998;114(3):713–22.
- Flores RM, Akhurst T, Gonen M, et al., Positron emission tomography defines metastatic disease but not locoregional disease in patients with malignant pleural mesothelioma, J Thorac Cardiovasc Surg, 2003;126(1):11–16.
- Flores RM, Diffuse Malignant Mesothelioma, 6th edition, New York: Lippencott Williams & Wilkins, 2005.
- Boutin C, Rey F, Thoracoscopy in pleural malignant mesothelioma: a prospective study of 188 consecutive patients. Part 1: Diagnosis, Cancer, 1993;72(2):389–93.
- Rusch VW, A proposed new international TNM staging system for malignant pleural mesothelioma. From the International Mesothelioma Interest Group, Chest, 1995;108(4):1122–8.
- Curran D, Sahmoud T, Therasse P, et al., Prognostic factors in patients with pleural mesothelioma: the European Organization for Research and Treatment of Cancer experience, J Clin Oncol, 1998;16(1):145–52.
- Herndon JE, Green MR, Chahinian AP, et al., Factors predictive of survival among 337 patients with mesothelioma treated between 1984 and 1994 by the Cancer and Leukemia Group B, Chest, 1998;113(3):723–31.
- Maziak DE, Gagliardi A, Haynes AE, et al., Surgical management of malignant pleural mesothelioma: a systematic review and evidence summary, Lung Cancer, 2005;48(2):157–69.
- Vogelzang NJ, Rusthoven JJ, Symanowski J, et al., Phase III study of pemetrexed in combination with cisplatin versus cisplatin alone in patients with malignant pleural mesothelioma, J Clin Oncol, 2003;21(14):2636–44.
- Flores RM PH, Venkatraman E, et al., Extrapleural Pnuemonectomy (EPP) versus Pleurectomy/Decortication (PD) in the surgical management of malignant pleural mesothelioma (MPM): results in 663 patients, The American Association for Thoracic Surgery 87th Annual Meeting, 2007.
- Alberts AS, Falkson G, Goedhals L, et al., Malignant pleural mesothelioma: a disease unaffected by current therapeutic maneuvers, J Clin Oncol, 1988;6(3):527–35.
- Holsti LR, Pyrhonen S, Kajanti M, et al., Altered fractionation of hemithorax irradiation for pleural mesothelioma and failure patterns after treatment, Acta Oncol, 1997;36(4):397–405.
- Law MR, Gregor A, Hodson ME, et al., Malignant mesothelioma of the pleura: a study of 52 treated and 64 untreated patients, Thorax, 1984;39(4):255–9.
- Ruffie P, Feld R, Minkin S, et al., Diffuse malignant mesothelioma of the pleura in Ontario and Quebec: a retrospective study of 332 patients, J Clin Oncol, 1989;7(8):1157–68.
- Boutin C, Rey F, Viallat JR, Prevention of malignant seeding after invasive diagnostic procedures in patients with pleural mesothelioma. A randomized trial of local radiotherapy, Chest, 1995;108(3):754–8.
- Berghmans T, Paesmans M, Lalami Y, et al., Activity of chemotherapy and immunotherapy on malignant mesothelioma: a systematic review of the literature with meta-analysis, Lung Cancer, 2002;38(2):111–21.
- Broomfield S, Currie A, van der Most RG, et al., Partial, but not complete, tumor-debulking surgery promotes protective antitumor memory when combined with chemotherapy and adjuvant immunotherapy, Cancer Res, 2005;65(17):7580–84.
- Steele JP, Shamash J, Evans MT, et al., Phase II study of vinorelbine in patients with malignant pleural mesothelioma, J Clin Oncol, 2000;18(23):3912–17.
- Mintzer DM, Kelsen D, Frimmer D, et al., Phase II trial of high-dose cisplatin in patients with malignant mesothelioma, Cancer Treat Rep, 1985;69(6):711–12.
- Sugarbaker DJ, Flores RM, Jaklitsch MT, et al., Resection margins, extrapleural nodal status, and cell type determine post-operative long-term survival in trimodality therapy of malignant pleural mesothelioma: results in 183 patients, J Thorac Cardiovasc Surg, 1999;117(1):54–63.
- Rusch VW, Venkatraman ES, Important prognostic factors in patients with malignant pleural mesothelioma, managed surgically, Ann Thoracic Surg, 1999;68(5):1799–804.
- de Perrot M, Uy K, Anraku M, et al., Impact of lymph node metastasis on outcome after extrapleural pneumonectomy for malignant pleural mesothelioma, J Thorac Cardiovasc Surg, 2007;133(1):111–16.
- Rusch VW, Rosenzweig K, Venkatraman E, et al., A phase II trial of surgical resection and adjuvant high-dose hemithoracic radiation for malignant pleural mesothelioma, J Thorac Cardiovasc Surg, 2001;122(4):788–95.
- Allen AM, Czerminska M, Janne PA, et al., Fatal pneumonitis associated with intensity-modulated radiation therapy for mesothelioma, Int J Radiat Oncol Biol Phys, 2006;65(3):640–45.
- Weder W, Kestenholz P, Taverna C, et al., Neoadjuvant chemotherapy followed by extrapleural pneumonectomy in malignant pleural mesothelioma, J Clin Oncol, 2004;22(17): 3451–7.
- Flores RM, Krug LM, Rosenzweig KE, et al., Induction chemotherapy, extrapleural pneumonectomy, and post-operative high-dose radiotherapy for locally advanced malignant pleural mesothelioma: a phase II trial, J Thorac Oncol, 2006;1(4):289–95.
- Weder W, Stahel R, Bernhard J, et al., Multicenter trial of neo-adjuvant chemotherapy followed by extrapleural pneumonectomy in malignant pleural mesothelioma, Ann Oncol, 2007;18(7):1196–202.
- Krug L PH, Rusch VW, et al., A multicenter US trial of neoadjuvant pemetrexed plus cisplatin (PC) followed by extrapleural pneumonectomy (EPP) and hemithoracic radiation (RT) for stage I–III malignant pleural mesothelioma (MPM). ASCO Annual Meeting, 2007, J Clin Oncol, 2007;7561.
- Garland LL, Rankin C, Gandara DR, et al., Phase II study of erlotinib in patients with malignant pleural mesothelioma: a Southwest Oncology Group Study, J Clin Oncol, 2007;25(17): 2406–13.
- Govindan R, Kratzke RA, Herndon JE 2nd, et al., Gefitinib in patients with malignant mesothelioma: a phase II study by the Cancer and Leukemia Group B, Clin Cancer Res, 2005;11(6): 2300–2304.
- Mathy A, Baas P, Dalesio O, van Zandwijk N, Limited efficacy of imatinib mesylate in malignant mesothelioma: a phase II trial, Lung Cancer, 2005;50(1):83–6.
- Karrison T, Kindler HL, Gandara DR, et al., Final Analysis of a multi-center, double-blind, placebo-controlled, randomized phase II trial of gemcitabine/cisplatin (GC) plus bevacizumab (B) or placebo (P) in patients with malignant mesothlioma (MM), J Clin Oncol, 2007;25:7526.
- Baas P, Boogerd W, Dalesio O, et al., Thalidomide in patients with malignant pleural mesothelioma, Lung Cancer, 2005;48(2): 291–6.
- Jahan T GL,Wang X, et al., Vatalanib in patients with previously untreated advanced malignant mesothelioma (MM): Preliminary analysis of a phase II study by the Cancer and Leukemia Group B (CALGB 30107), Lung Cancer, 2005;49(Suppl. 2):222a.
- Fenell D, Porta C, et al., Proteasome inhibitors for treatment of malignant mesothelioma, Lung Cancer, 2006;54(Suppl. 1):50a.
- Krug LM, Curley T, Schwartz L, et al., Potential role of histone deacetylase inhibitors in mesothelioma: clinical experience with suberoylanilide hydroxamic acid, Clin Lung Cancer, 2006;7(4): 257–61.
Further Resources

Trending Topic
It is with great pleasure that we present the latest edition of touchREVIEWS in Oncology & Haematology. This issue highlights the remarkable progress and innovation shaping the fields of oncology and haematology, featuring articles that delve into both emerging therapies and the evolving understanding of complex malignancies. We open with an editorial by Mohammad Ammad […]
Related Content in Lung Cancer
Highlights Immunotherapy, especially combinatory immunotherapy, has shown promise with prolonged survival for patients with advanced mesothelioma in the first-line setting (see the sections on ‘Systemic treatment and immunotherapy debut’ and ‘Randomized immunotherapy trials of mesothelioma’). Histology-based therapy is important to ...

Welcome to the latest issue of touchREVIEWS in Oncology & Haematology. We are honoured to present a series of compelling articles that reflect cutting-edge developments and diverse perspectives in this ever-evolving field. This issue includes a series of editorials and ...

Unmet clinical needs for patients with advanced epidermal growth factor receptor-mutated non–small-cell lung cancer Epidermal growth factor receptor (EGFR)-tyrosine kinase inhibitors (TKIs) have become the standard first-line therapy for patients with advanced non–small-cell lung cancer (NSCLC) harbouring ...

Accurately detecting lung tumours and their margins is important for disease outcomes.1,2 However, detection is challenging due to the use of minimally invasive surgery and current localization techniques, such as computed tomography (CT)-guided and endobronchial interventions, which add significantly ...
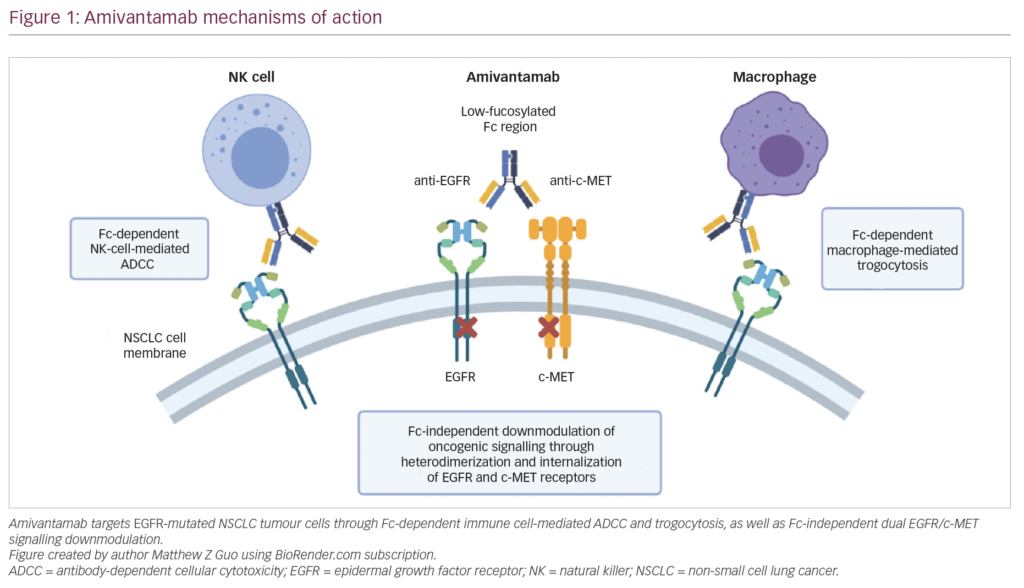
Cancer treatment has expanded rapidly in recent years as advancements in the fields of tumour biology and molecular diagnostics have informed the development of targeted therapies, improving survival in patients with oncogene-addicted cancers with therapeutically relevant molecular lesions. Osimertinib has ...
The treatment of patients with non-small cell lung cancer (NSCLC) has seen significant advances in the past decade, with the availability of multiple targeted therapy agents for oncogenic-driven non-squamous NSCLC and the advent of immunotherapy that has completely revolutionized the ...
Advanced non-small cell lung carcinoma (NSCLC) treatment paradigms have evolved during the past decade. Identification of tumor-specific molecular alteration in cancer driver genes has led to the development of targeted therapies.1–3 Most of the tumors harboring such alterations are sensitive ...
Radiation-induced esophagitis, caused by incidental damage to the mucosal lining of the esophagus during radiation therapy, is a common and clinically important toxicity in patients with lung cancer. Esophagitis generally develops 2–3 weeks after initiation of radiation therapy and presents as ...
Historically, chemotherapy represented the only available treatment for patients with advanced non-small-cell lung cancer (NSCLC) who did not show any target molecular driver, such as epidermal growth factor receptor (EGFR), anaplastic lymphoma kinase (ALK) or the receptor tyrosine kinase ROS1. ...

At initial diagnosis of metastatic disease, central nervous system (CNS) metastases are present in 22–33% of patients with anaplastic lymphoma kinase (ALK)-rearranged (ALK+) non-small cell lung cancer (NSCLC). After crizotinib failure, the incidence can reach up to 70%, compared with 40% in ...
Non-small cell lung cancer (NSCLC) remains a world-wide health issue, accounting for 85% of all lung cancers, of which there were an estimated 2.1 million new cases and 1.76 million deaths in 2018; equivalent to 11.6% of the global cancer burden.1,2 This incidence is expected ...

Welcome to the fall edition of Oncology and Hematology Review (US), which features a wide variety of articles covering topics of interest to oncologists and hematologists, as well as the wider medical community. We begin with some expert interviews, which ...
Latest articles videos and clinical updates - straight to your inbox
Log into your Touch Account
Earn and track your CME credits on the go, save articles for later, and follow the latest congress coverage.
Register now for FREE Access
Register for free to hear about the latest expert-led education, peer-reviewed articles, conference highlights, and innovative CME activities.
Sign up with an Email
Or use a Social Account.
This Functionality is for
Members Only
Explore the latest in medical education and stay current in your field. Create a free account to track your learning.

