Abstract
In the light of the modest activity of unselected treatment of non-small-cell lung cancer (NSCLC), therapeutic targets and biomarkers are urgently needed. Many attempts have been undertaken to find prognostic and predictive markers in NSCLC. To date only histology, i.e. squamous versus non-squamous, and activating epidermal growth factor receptor mutations have entered clinical practice as biomarkers. Excision-repair cross-complementation group I-protein (ERCC1), ribonucleotide reductase regulatory subunit M1 (RRM1) and echinoderm microtubule-associated ligand-anaplastic lymphoma kinase (EML4-ALK) are possible future options as well as genetic signatures. This article covers these relevant matters.
Support: The publication of this article was funded by F Hoffmann-La Roche. The views and opinions expressed are those of the author and not necessarily those of F Hoffmann-La Roche.
Despite advances in the management of non-small-cell lung cancer (NSCLC), including the introduction of molecularly targeted therapies such as epidermal growth factor receptor (EGFR) tyrosine kinase inhibitors (TKIs), many patients do not obtain sustained benefit from cytotoxic agents or newer targeted therapies. Personalising therapy to select those most likely to benefit from a particular treatment approach promises to limit toxic effects and maximise efficacy instead of following the ‘trial and error’ principle that we practice today in the majority of patients. Therefore, reliable biomarkers to select treatments for patients most likely to obtain benefit have been an important focus for many research groups. Several molecular markers have been identified that could serve as predictors of improved outcome with targeted or cytotoxic therapies in NSCLC (see Table 1); however, only EGFR mutations, which are positive predictors of response and improved progression-free survival (PFS) following EGFR-TKI treatment, are ready for widespread use. Therefore, there are still significant challenges to implement predictive biomarker analyses in clinical practice.
Biomarkers – Prognostic versus Predictive
A prognostic marker is a characteristic that has a positive or negative effect on a patient’s outcome, regardless of the treatment they receive. A predictive marker is a characteristic that renders a patient either more or less likely to respond to a particular type of treatment or a specific agent. A typical pure prognostic marker is performance status.1 The worse the condition of a patient is, the poorer the prognosis is. A marker with predictive properties (although it is prognostic too) is an activating EGFR mutation detected in the tumour tissue. It predicts better response rates and PFS when treated with gefitinib or erlotinib compared with wild-type EGFR, at least in first-line treatment.2,3 However, activating EGFR mutations also have a prognostic impact,4,5 which can also be seen in the control arms of randomised studies of EGFR-TKI in patients with activating mutations: they have a favourable survival compared with patients with wild-type EGFR.6
Another approach to determining prognosis in NSCLC is the use of gene signatures. In the early stages of disease they might predict recurrence and thereby stratify high- and low-risk groups. The former might benefit from adjuvant chemotherapy and the latter might suffice with observation only. The lung metagene model is an approach comparing gene-expression patterns. A metagene is a cluster of genes. In a training cohort consisting of 89 tumour-resection samples from early-stage NSCLC, whole RNA was extracted and a gene-expression profile was made out of each tumour. Because the clinical courses of the patients were known, predictions of recurrence were made, based on the metagenes, taking classic prognostic factors (age, sex, tumour diameter, stage, histological subtype and smoking history) into account. Disease-free survival at five years was set at 0 and death within 2.5 years after diagnosis as 1. In two validation cohorts the metagene model was verified. Indeed, the model had a predictive accuracy of >70% in both validation cohorts, which is much better than clinical prognostic factors alone.7 However, this approach is complex and expensive and thereby not feasible for clinical practice to date. Later, Chen and colleagues identified five genes that could identify high-risk patients for relapse. Depending on the cohort they had a 2.82–4.36-fold higher risk of death from any cause compared with patients whose tumours did not express this signature.8 This approach might be more feasible than the metagene approach; however, a trial dealing with tailored therapy according to the genetic signature is not yet published. One possible design proposed by Potti et al. is to stratify by the genetic signature and to randomise high-risk patients to observation or adjuvant chemotherapy.7
Markers to Tailor Chemotherapy
Adjuvant chemotherapy is an accepted standard treatment for patients with stage II/IIIa NSCLC. However, the overall survival (OS) benefit is modest at best, resulting in an overall 5.4% survival benefit after five years.9 To improve these results, a predictive marker is needed to avoid unnecessary chemotherapies in patients who have a low probability of benefit. Such a marker is the excision-repair cross-complementation group I-protein (ERCC1), which repairs platinum-induced DNA-damage. In its presence, platinum based chemotherapy may not work. This was shown in a subset of patients from the International Adjuvant Lung Trial (IALT) where ERCC1 was retrospectively measured by immunohistochemistry (IHC) in tumour specimens. It could be shown that only patients whose tumours did not express ERCC1 had a benefit from chemotherapy (hazard ratio [HR] 0.65; p=0.002), whereas those with ERCC1-expression had no benefit and even a numerical trend towards a worse outcome (HR 1.14; p=0.4).10 Major drawbacks of this study were the facts that these findings were never confirmed in a prospective trial and that the measurement by IHC was prone to error and interobserver variability (0, +, ++ and +++, respectively).
In advanced stages of disease, a randomised trial stratifying by ERCC1 status was conducted by Cobo and colleagues: 366 patients were randomised into a control arm and a ‘genotypic arm’ in a 1:2 ratio. In the genotypic arm, ERCC1 was measured by a polymerase-chain reaction (PCR)-based method and patients were further stratified into a high genotypic group consisting of patients with high ERCC1 levels and a low genotypic group with low levels. The former received a platinum-free regimen consisting of docetaxel and gemcitabine whereas the low genotypic group received docetaxel and cisplatin as did the control group. The primary end-point was the response rate. And indeed, in the genotypic group, the response rates were significantly higher with 53.2% in the low genotypic group and 47.2 in the high genotypic group (averaged 51.2%) compared with 39.3% in the control group (p=0.02 for average versus control). However, this did not translate into an OS benefit with OS being 9.82 (95% confidence interval [CI] 8.9–10.7) months in the control group versus 9.80 (95% CI 8.7–10.9) months in the genotyped group.11 So it is still doubted whether ERCC1 will ever be used to tailor chemotherapy in NSCLC.
Pemetrexed, a multi-targeted antifolate, is one of the newer cytotoxic agents to treat NSCLC. In a randomised trial it was compared to gemcitabine as a combination partner of cisplatin in first-line treatment of advanced NSCLC. The trial had a non-inferiority design and the primary end-point was OS. There was a pre-specified subgroup analysis to test the assumption that patients with non-squamous histology will have a favourable OS with pemetrexed. And indeed, in the overall patient population there was no difference between the regimens (median OS 10.3 months in both groups), whereas in the non-squamous-group, OS benefit was greater following pemetrexed/cisplatin (11.8 months [95% CI 10.4–13.2]) compared with gemcitabine/cisplatin (10.4 months [95% CI 9.6–11.2]), resulting in a HR of 0.81 (95% CI 0.70–0.94). In patients with squamous cell NSCLC, OS time was longer in patients receiving gemcitabine/cisplatin compared with cisplatin/pemetrexed (10.8 versus 9.4 months, HR 1.23 [95% CI 1.00–1.51]; p=0.05).12 There are other studies showing, that pemetrexed does not work well in patients with squamous-cell NSCLC13 and in small-cell lung cancer.14 The driver behind this might be a biomarker: thymidylate synthase (TS). There may be a negative correlation between TS and pemetrexed efficacy because we know that TS levels are higher in squamous-cell NSCLC than in adenocarcinomas.15 However, this has never been proved by a trial that prospectively stratifies for a TS level.
Another possible biomarker is ribonucleotide reductase regulatory subunit M1 (RRM1). Lee et al. retrospectively collected 40 formalin-fixed, paraffin-embedded NSCLC tissues from patients treated with gemcitabine. They investigated the protein expression of RRM1 by IHC. RRM1 expression was positive in 14 (35%) and negative in 26 (65%) cases. Ten patients (25%) were treated as first-line and 30 (75%) patients as second-line. The OS of RRM1-positive groups was significantly shorter than RRM-negative groups (5.1 versus 12.9 months; p=0.022). The response rates of 38 out of 40 patients were assessable. Disease control rate (PR + SD) of the RRM1-positive groups was significantly lower than that of RRM1-negative groups (23 versus 56%; p=0.053).16 This suggests that RRM1 expression is a negative predictor of gemcitabine efficacy but seems to have prognostic impact too.17 Again, no prospective RRM-1 tailored trial has been published.
Biomarkers for Targeted Therapy
Targeted therapy mostly consists either of small molecules (ending on ‘ib’) or monoclonal antibodies (ending on ‘mab’), targeting specific pathways in cancer growth. The only approved drugs in NSCLC are the EGFR-TKI gefitinib for patients harbouring an activating EGFR mutation as well as erlotinib in unselected NSCLC in second- or third-line treatment and as first-line maintenance therapy. The anti-VEGF antibody bevacizumab is approved for first-line treatment of advanced non-squamous NSCLC in combination with carboplatin and paclitaxel. The following section will focus on approved drugs but will take into account crizotinib, which is a drug showing promising results in a subset of NSCLC patients (see below).
For VEGF antibodies, no predictive biomarkers are available yet. The development of hypertension – due to drug-induced nitric oxide depletion and vascular rarefication – during treatment was associated with a favourable outcome in a retrospective study.18 However, treatment-induced hypertension is not predictive because therapy has already begun; no other biomarkers for the prediction of treatment success with bevacizumab exist.
One condition for the success of targeted therapy is the presence of an upregulated pathway (the so-called ‘driver mutation’), which the cancer cell is addicted to (‘oncogene addiction’). In East Asian never-smoking patients with lung adenocarcinoma, 90% harbour a known driver mutation in a series of 52 patients: EGFR in 78.8%, EML4-ALK in 5.8%, HER2 in 3.8 and kRAS in 1.9%.19 These mutations can be considered to be biomarkers for the prediction of therapeutic success of targeted therapy. Interestingly, these driver mutations seem to exclude each other with only anecdotal case reports of concurrent appearance. Some authors proposed sequential testing unless a test is positive.20 However, we do not know why these mutations should exclude each other, so I would not support this sequential approach of testing. The only targets to date with a therapeutic consequence are EGFR activating mutations and echinoderm microtubule-associated ligand-anaplastic lymphoma kinase (EML4-ALK).
Although EGFR-TKIs have a moderate effect in wild-type NSCLC in subsequent therapies,6,21 patients with activating EGFR mutations in first-line therapy have the highest benefit2,3 in terms of response and PFS from these drugs. Therefore, the activating EGFR mutation is the only biomarker yet introduced into clinical practice. EGFR mutations are detected in tumour-tissue blocks with PCR-based methods and/or direct sequencing as described elsewhere.22 Another technique, fluorescent in situ hybridisation (FISH) visualises aberrant gene-copy numbers but has lower sensitivity than PCR. IHC staining for EGFR can only detect overexpression, not mutation. Mutation-specific monoclonal antibodies against L858R and Del19 mutations have a sensitivity of 100% and 71–85%, respectively.23 These antibodies may become a screening tool, however they only cover these two mutations.
In summary, sequencing remains the gold standard. A major challenge is the fact that tumour tissue is not readily available in every lung cancer patient. So there are attempts to detect EGFR mutations in cytological specimens in as few as eight cancer cells24 or even in circulating tumour cells in blood.25 However, these techniques have not been prospectively validated yet.
Although PFS is significantly longer than with conventional chemotherapy, almost every patient with an activating EGFR mutation treated with an EGFR-TKI will experience disease progression eventually – a situation known as ‘acquired resistance’.26 One reason for this is an upcoming resistance mutation in Exon 20, T790M. It is not clear whether this mutation develops in the course of the disease or if it is present in a small clone of tumour cells from the beginning, continuously overgrowing the sensitive cell lines over time. No prospective trials on the treatment of T790M mutations exist, however irreversible EGFR-TKI may be effective drugs against tumours with this mutation.27 Another cause of acquired resistance is the amplification of another pathway, cMet, which acts parallel to EGFR. Although IHC is available for cMet and active drugs may appear, it is far from being a standard biomarker.28–30
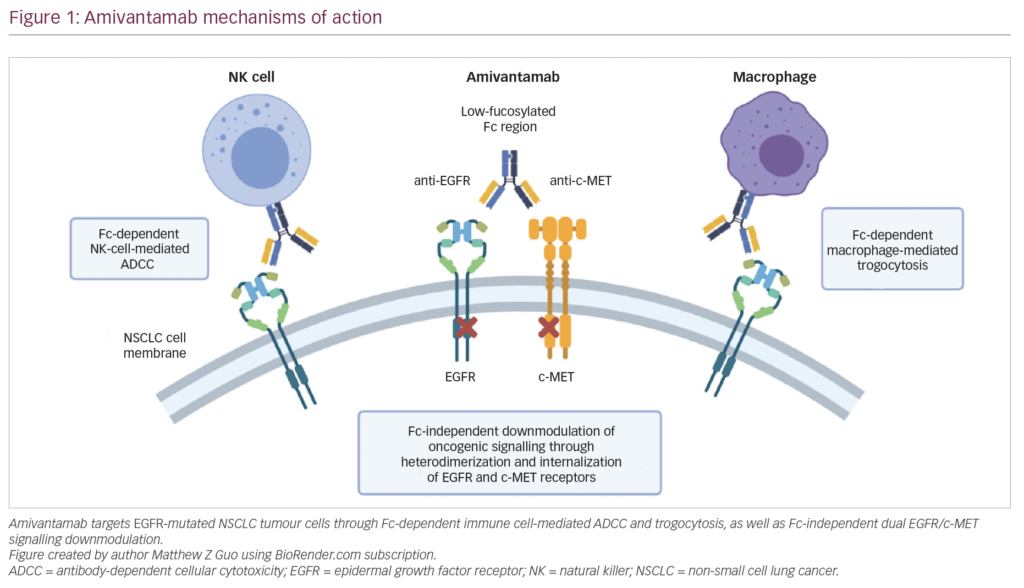
Another driver mutation in human cancer is the translocation of EML4 and ALK. This is a small inversion on chromosome 2. The transcription product is a constitutionally activated kinase which can be blocked by the small molecule crizotinib. In a phase I/II study, patients with tumours harbouring an EML4-ALK translocation achieved a response rate of 57% despite numerous previous therapies. Median PFS has not been reached by the time of publication with a six-months PFS-probability of 72% (95% CI 61–83%).31 The detection of the translocation is performed by FISH analysis detecting a translocation in the ALK gene (see Figure 1). If >15% of tumour cells harbour such a ‘split signal’, the test is deemed positive. FISH is prone to error, because the threshold of 15% is somewhat arbitrary and if the two parts of ALK are too close to each other they are not recognised as a split signal. IHC with a specific antibody can be performed from tumour tissue. However, the test is not commercially available. PCR-based techniques are also available. To date it is not clear which test is going to be the gold standard.
Conclusion and Future Perspectives
To date, very few biomarkers have entered clinical practice: histology as an indicator for pemetrexed activity, EGFR activating mutations for efficacy of EGFR-TKIs and maybe in the near future EML4-ALK for sensitivity to crizotinib. At least in never-smoking patients with adenocarcinoma these two driver mutations should be searched for. A major challenge will continue to be sufficient tissue acquisition in NSCLC because diagnosis is often established from small biopsies or even cytologies only (see Figure 2). This leads to two problems: does a small biopsy reflect the biology of the whole tumour, because NSCLC tumours tend to be heterogeneous?32 And, is there enough material for multiple molecular tests? A major step forwards would be analyses based on circulating tumour cells; however, this cannot be achieved in the near future.