At least two-thirds of patients suffering from advanced cancer report persistent (background) pain, described as pain lasting for 12 or more hours per day.1 Relief of chronic cancer-related pain is achieved adequately in a majority of cancer patients with analgesic medications that are administered on a fixed schedule following World Health Organization (WHO) guidelines.1–3 However, in addition to persistent and otherwise well-controlled background pain, generally, one-half to two-thirds of patients may also experience episodes of significant and severe pain that ‘breaks through’ the around-the-clock analgesia.4,5 Breakthrough pain is a common feature in patients with cancer and is associated with significant physical, psychologic, and economic burdens on patients as well as their carers. This article aims to provide an overview of breakthrough pain and the associated clinical features, and to examine the evidence for the impact of breakthrough pain on cancer patients, their carers and the healthcare system. A key principle in medicine is to make the correct diagnosis to allow for adequate assessment followed by effective treatment. Although breakthrough pain is now well recognized as an issue in cancer pain management, effective diagnosis and treatment of breakthrough pain is often not realized, in part due to differences in breakthrough pain definitions as well as historically inadequate treatments based on opioids.4–7
Breakthrough Pain—Definition and Prevalence
Breakthrough pain was first defined by Portenoy and Hagen as “a transitory exacerbation of pain that occurs on a background of otherwise stable pain in a patient receiving chronic opioid therapy”.6 This definition of breakthrough pain has since been broadened to include patients with non-malignant pain disorders and patients with or without background pain medication.7–9 Despite there being no universal agreement on the definition of breakthrough pain, the Association for Palliative Medicine of Great Britain and Ireland most recently defined it as “a transient exacerbation of pain that occurs either spontaneously, or in relation to a specific predictable or unpredictable trigger, despite relatively stable and adequately controlled background pain”, which takes into account predictable (volitional) or unpredictable (involuntary) trigger factors.10 Breakthrough pain can occur at all stages of cancer in adults although its presence is more common when the disease is at an advanced stage and where the patient has a poor performance status.11 Breakthrough pain is generally acute in onset (reaching maximum severity within three minutes) and short in duration (the average duration of pain episodes is about 30 minutes, with a range of between 1–240 minutes).12,13 Breakthrough pain can happen unexpectedly and for no obvious reason, or it may be initiated by coughing, moving, or going to the bathroom. A great variation in the frequency of breakthrough pain episodes has been reported (possibly due to the use of different definitions of breakthrough pain) and multiple breakthrough pain episodes a day are common.5–7,14 The average number, however, is four to six episodes per day.6,14 Studies have reported a breakthrough pain prevalence in cancer patients of between 40–86%;3,6,11,13–17 prevalence varies depending on the breakthrough pain definition used and also the patient populations that are selected for study (e.g. ambulatory patients treated in community practices versus hospice-treated patients).18,19 The clinical features of breakthrough pain vary from individual to individual and may vary within an individual over time.
Breakthrough Pain Subtypes and Clinical Features
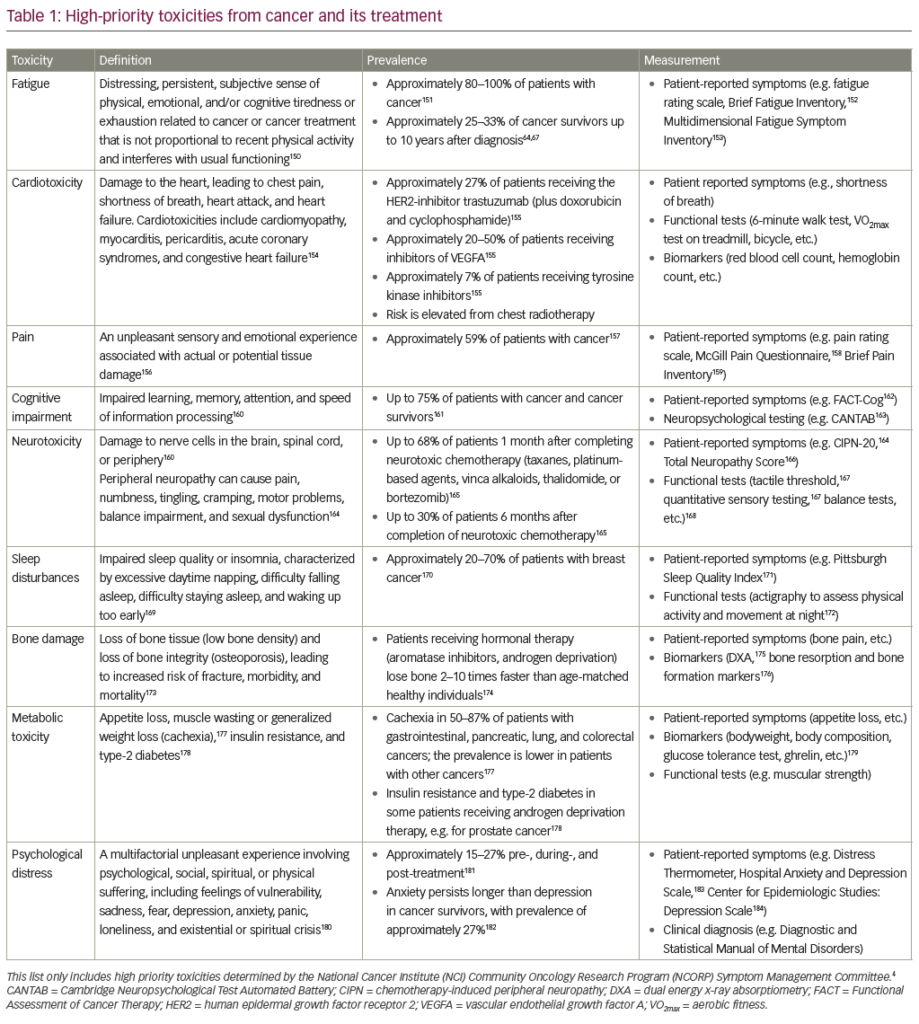
The breakthrough pain experienced by most patients can usually be classified into one of three subtypes: incident-predictable, incidentunpredictable, and idiopathic (spontaneous). Each of the three subtypes is summarized in Table 1. End-of-dose failure consistently occurs just prior to the next scheduled dose of around-the-clock analgesia and is due to an inadequate analgesic dose or a too-lengthy administration interval. This is not considered as breakthrough pain as baseline pain is (by definition) not controlled by the optimum dose of around-the-clock medication.6,13,14
The most common subtype (accounting for about half of breakthrough pain episodes) is incident pain, which is typically triggered by musculoskeletal movements and due to bone metastases.7 Incident pain may be predictable when precipitated by volitional factors (e.g. movement), or unpredictable when precipitated by nonvolitional factors (e.g. bladder spasm, coughing). Idiopathic pain flares in the absence of a specific trigger and occurs randomly and unpredictably, making management difficult. No cause is evident in 27–38% of breakthrough pain episodes. However, precipitating factors, such as movement, are identified in 55–80% of episodes.3,15
The causes of breakthrough pain vary in different patients. Up to 4% of breakthrough pain episodes are of uncertain cause and may be related to comorbidities such as arthritis, whereas studies have shown that 67–76% of pains are due to the neoplasm and 20–33% are due to the treatment.4,14
Breakthrough pain mechanisms are nociceptive, neuropathic, or mixed. Nociceptive somatic pain involves somatic structures such as muscle and bone and can be described as aching or throbbing. Nociceptive visceral pain arises from underlying solid or hollow viscus and is described as squeezing, gnawing, or cramp-like pain. Visceral pain is not well-localized and can have referral pain to somatic structures. Neuropathic pain involves central or peripheral nervous system damage and is described as burning or stabbing. Nociceptive breakthrough pain affects 38–53% of patients, while neuropathic pain affects 10–54% and mixed pain 20–52% of patients who have pain.4,13,14,20
Impact of Breakthrough Pain on Patients
Without treatment, flares of breakthrough pain impair a person’s sense of wellbeing, interfere with daily activities, interrupt disease-related treatment schedules, result in appetite loss, sleeping disturbances, anxiety, and depression, and renders the treatment of persistent background pain more difficult. As fear of breakthrough pain events grow, patients tend to remain sedentary and socially isolated, thus exacerbating physical de-conditioning, pain-related disability, and causing psychosocial disability.20,21
In addition, poorly controlled, or even fully uncontrolled pain is related to dissatisfaction with opioid therapy, and poor medical outcomes.22 This makes it more difficult for physicians to manage chronic pain as poorly controlled breakthrough pain will lead to aberrant opioid use, particularly with immediate-release and rapid-onset opioid formulations. Because of addiction fears, many chronic pain patients are not compliant, hence pain remains unrelieved and the adverse effects on quality of life are therefore significant.23 Quality of Life
It is clear from a recent survey that breakthrough pain has a marked impact on a patient’s quality of life. In a pan-European survey of cancer-related pain across 12 countries, 2,864 cancer patients completed a screening interview and rated their pain to be ≥5 on a validated numerical rating scale of zero to 10 (where zero is no pain at all and 10 is the worst pain imaginable) several times a month or more. Of 573 patients randomly selected for the second phase in-depth interview, 77% were receiving prescription-only analgesics with 63% of these patients experiencing breakthrough pain. Only 48% of the surveyed patients (n=573) reported a good quality of life, with 51% suffering from pain that impaired thinking or concentrating, 69% had difficulty in performing normal activities in daily life, and 43% felt like a burden to others. Almost one in three patients reported being in so much pain that they were unable to care sufficiently for themselves or others, while 32% reported feeling so bad that they did not want to live.5
Patients with uncontrolled breakthrough pain are often less satisfied with their analgesic therapy, have decreased function because of their pain, and more often experience adverse social and psychosocial consequences, such as increased levels of anxiety and/or depression.6,24 Depression is also clearly associated with chronic pain.5,25 Cancer patients with breakthrough pain typically experience more depression and anxiety and report a worse impact of pain on their quality of life compared to cancer patients who do not have breakthrough pain.14
Costs
Patients and caregivers can expect direct, indirect, and intangible costs as a result of breakthrough pain. This includes increased prescription costs, more breakthrough pain-related visits to healthcare professionals, and more hospitalizations, as well as costs relating to child care, alternative pain relief methods, psychotherapy, loss of earnings, and stress and strain on family members.26
Effective treatment of breakthrough pain is not only good medical practice but is also cost-effective by decreasing the use of medical resources.20,27 In a survey conducted in 160 cancer patients, patients with cancer-related breakthrough pain used more healthcare resources, reported more hospitalizations related to pain relief (1.0 versus 0.4 per year among patients without breakthrough pain), experienced longer hospital stays per event (7.1 versus 4.1 days), undertook more emergency department visits, and paid greater treatment costs than those without breakthrough pain.20 Evidence from a subsequent study by Dr Fortner et al. colleagues strengthens the argument that good clinical management of breakthrough pain will significantly decrease pain-related costs.28
Breakthrough Pain Assessment
Cancer-related breakthrough pain has such an adverse consequence on quality of life that it is imperative that a broad ranging and complete assessment take place before choosing the most appropriate treatment option. An effective and comprehensive assessment will lead to successful management in most circumstances, which is defined as adequate breakthrough pain relief as well as reduced medical costs. A comprehensive assessment includes defining the important characteristics of the breakthrough pain incidents as well as characterizing any associated factors, such as response to interventions and analgesics and the presence of any exacerbating or relieving factors. A complete picture of the breakthrough pain for each individual patient will then be developed, resulting in the appropriate treatment based on the patient’s symptoms.10 Cancer breakthrough pain is assessed using pain questionnaires and patient-related instruments as outlined in a number of studies during the last three decades. Validated questionnaires ask questions about various characteristics of pain, including the temporal patterns, severity and location of the pain, the relationship to the regularly scheduled analgesic, precipitating events, mechanism and etiology, and palliative factors.6,11,13,29 Such questionnaires are usually structured within an interview and assessed in combination with medical records in order to identify the cause and pathophysiology of breakthrough pain.14 The following instruments are used when assessing pain and its impact on the patient.
- The Memorial Pain Assessment Card (MPAC)—This measures pain and global mood (psychologic distress) using three 100mm visual analog scales (VAS) including pain intensity, pain relief, and mood. It also includes an eight-item verbal rating scale. The instrument has been validated in the cancer population.30
- The Brief Pain Inventory (BPI)—This is a widely used tool to assess pain intensity and interference with activity, mood, social relations, walking, work, sleep, and overall enjoyment of life. A numerical zero to 10 scale is used, where zero means no pain and 10 means worst pain possible. A seven-item subscale of BPI evaluates the degree to which pain interferes with function and quality of life. Each activity is assessed on a zero to 10 numeric scale, where zero means no interference and 10 means complete interference. This subscale, which has been extensively validated in the cancer population, provides a global measure of pain-related interference.31–33
- The Beck Depression Inventory (BDI)—This is a 21-item self-reporting instrument designed to measure the symptoms associated with depression. It is reliable and has two main factors; a cognitive factor, which accounts for most of the variance, and a vegetative factor.34
- The Beck Anxiety Inventory (BAI)—The BAI is a 21-item self-report instrument designed to measure the symptoms associated with anxiety. It is highly reliable and has two main factors; somatic symptoms, and subjective anxiety or panic symptoms.35
- The Karnofsky Performance Status Score (KPS)—This is an observer-rated measure of performance status. The score reflects the extent of the ability for physical functioning.36
- The Functional assessment of cancer therapy general scale (FACT-G)—This is a 28-item general patient-rated measure of quality of life. Each item is scored from zero, meaning not at all, to four, meaning very much.11,29
- The Memorial symptom assessment scale short form (MSAS-SF)—This survey includes a patient assessment for symptom frequency or distress for 32 highly-prevalent physical and psychologic symptoms.11,29
Following initiation or changes in the management of breakthrough pain, particularly with an opioid, adequate reassessment of the patient is important. The objectives of reassessment are to determine the efficacy and tolerability of the treatment, as well as any change in the nature of the breakthrough pain. Inadequate reassessment may lead to the continuance of ineffective and/or inappropriate treatment.37 The four ‘As’ of chronic pain treatment should be considered for guiding reassessment:
- analgesia;
- activities of daily living;
- adverse events; and
- aberrant drug-related behavior.38
Treatment
Although the clinical significance of breakthrough pain has been recognized for many years,6,39–43 a comprehensive approach to pain management (apart from supplemental opioid use) has been absent until recently. It is only in recent years that drugs targeted to breakthrough pain and novel routes of administration have been studied for the expressed purpose of relieving breakthrough pain. General management guidelines aimed at reducing the intensity, severity, and impact of pain have been proposed recently.44 These guidelines emphasize the importance of comprehensive pain assessment and also highlight the positive outcomes that are possible with lifestyle changes (coping strategies), management of reversible causes (e.g. incident pain precipitant factors), modification of pathologic mechanisms (e.g. with anti-neoplastic therapies) and also pharmacologic or non-pharmacologic management of breakthrough pain.
Non-pharmacologic Treatment
The initial treatment of breakthrough pain should begin with non-pharmacologic interventions unless the pain episodes are especially severe or frequent.45 Lifestyle changes, such as the limitation of or increase in physical activities is considered. Other approaches, such as hypnosis and relaxation methods, or alternative medical therapies, such as acupuncture, may be beneficial in some patients either alone or in combination with opioid therapy.46 Certain patients appear to benefit from psychologic techniques such as distraction.30 Empowerment of patients and the relative lack of side effects are some of the advantages to non-pharmacologic treatment of breakthrough pain. However, it is necessary to have specialized staff available to administer the treatments (e.g. acupuncture, hypnosis), which is not always possible.
Modification of Pathologic Processes
Modification of the pathologic process is the primary treatment of the underlying etiology of breakthrough pain. This treatment requires a variety of approaches. More interventional pain management methods include traditional spinal or local anesthetic approaches and radiofrequency ablation. They are generally useful in the treatment of persistent pain, but also sometimes in the treatment of breakthrough pain. Examples of anesthetic approaches include the use of chemical, neurolysis, and epidural catheter infusion of local anesthetics, opioids, and/or clonidine.14,47,48
Other examples of invasive treatment could include stereotactic radiotherapy to a painful lesion, surgical repair of a fractured bone, kyphoplasty, decompression of obstructed bowel, and administration of antibiotics for a localized infection.6 Percutaneous cordotomy is done in order to treat refractory incident pain from bone metastases. In addition, intrathecal phenol block and pituitary ablation have been used to treat refractory breakthrough pain. Midline myelotomy is performed for visceral pain. The results of these invasive procedures are not always successful and the risks of adverse events need to be considered.49
Pharmacologic Treatment
The goal of pharmacologic treatment is to reduce pain intensity and frequency. Analgesics should have a quick onset and short duration of action due to the rapid onset and short duration of breakthrough pain.7 Factors such as the degree of analgesia, daily life activities, adverse drug events, and risk of abuse should be taken into consideration when administering drugs to relieve breakthrough pain.38 The analgesics used should have a short enough half-life to avoid carry-over opioid toxicity and should not interact with the around-the-clock medication and should be easy to administer.7 A large variety of opioid and non-opioid medications are available for breakthrough pain. The major categories of these pharmacologic approaches are outlined in Table 2 but are examined in more detail in the accompanying article by Marco Pappagallo.
Conclusion
Breakthrough pain is heterogeneous in nature and will vary in frequency, intensity, onset, duration, and predictability among individuals. Successful management of cancer pain depends on a comprehensive assessment that must take into account both background and breakthrough pain patterns. Subsequent management involves a number of very different interventions. Although the main treatment of breakthrough pain in cancer patients receiving opioids is principally based on the use of opioids, preferentially with a short onset, other approaches are often needed to supplement opioids. Further research into the pathophysiology of breakthrough pain, methods of individual patient assessment and pharmacologic/non-pharmacologic treatment approaches is necessary. It is hoped that improvements in assessments and treatments will improve the life of cancer patients with regard to breakthrough pain. ■