Development and Registration of Biosimilars
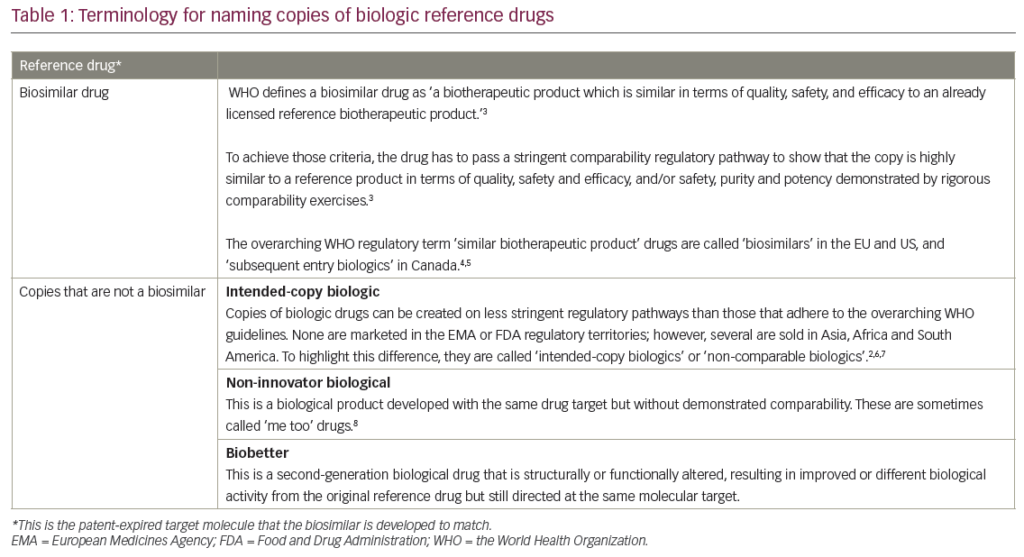
Biopharmaceuticals can now be marketed when the relevant patents have expired: they are therefore a subset of biopharmaceuticals with comparable safety and efficacy to originator reference products, referred to as biosimilars. The main difference between approved biosimilars and the reference product is that biosimilars will be less expensive. It is wellknown that drug costs account for an increasingly large proportion of expenditure in EU healthcare systems. The development of biosimilars provides a major opportunity for greater global access to affordable medicines.1 The European Medicines Agency (EMA) took a lead in providing a suitable regulatory process for the evaluation and approval of biosimilars; this has ensured that biosimilar approval is feasible and that approved biosimilars in the European Union (EU) are of appropriate quality. Biosimilars approved in the EU are evaluated according to criteria set out in a range of guidelines,2–4 which ensures the necessary safety and efficacy.
In Europe, biosimilar medicines must be approved by the EuropeanCommission (EC) through the European centralised procedure that is overseen by the regulatory body, the EMA. To gain approval, biosimilars have to be shown to be as safe and effective as the reference product. Potential concerns about immunogenicity, which applies to all biopharmaceuticals, whether reference products or biosimilars, are addressed through preclinical and clinical development programmes prior to approval, pharmacovigilance after approval and, if appropriate, through post-authorisation safety studies. The EMA grants marketing authorisation (MA) based on the EMA positive scientific opinion. With a transparent procedure, most data are made available to the public and are easily accessible on the EMA website.
The scope of trials required for registration of biosimilars is much broader than for generics. It is a stepwise procedure that begins with extensive analytical characterisation, followed by non-clinical trials priorto proceeding to clinical development, which includes pharmacokinetic (PK) and pharmacodynamics (PD) studies followed by clinical efficacy and safety trial(s).2 The quality factors relevant for demonstration of comparability for similar biological medicinal products containing recombinant DNA-derived proteins are addressed in the EMA guideline on similar biological medicinal products, 23 October 2014. Report No.: Committee for Medicinal Products for Human Use [CHMP]/437/04 Rev 1.4 Where applicable, product class specific annexes supplement this guideline, in this particular case (EMEA/CHMP/[Biosimilar Medicinal Products Working Party] BMWP/31329/2005).3
Granulocyte-colony Stimulating Factor Products Under Investigation
Neutropenia is a common adverse event (AE) during chemotherapy.5,6 In addition to the resultant risk of infection-related morbidity and mortality, patients developing severe (grade 3 or 4) or febrile neutropenia (FN) during chemotherapy often receive dose reductions and/or delays to their chemotherapy.5,6 Chemotherapy-induced neutropenia, leading to FN, usually requires immediate hospitalisation and administration of antibiotics and has been associated with increased healthcare costs7,8 and a reduced quality of life.9,10 Prevention of FN reduces hospital admissions, use of antibiotics and the requirement for dose reductions/ delays in chemotherapy.11–15
The European Guidelines Working Party of the European Organisation for Research and Treatment of Cancer (EORTC) have produced updated guidelines on the use of granulocyte-colony stimulatory factor (G-CSF) to reduce the incidence of chemotherapy-induced FN in adult patientswith lymphoproliferative disorders and solid tumours.5 According to the EORTC guideline, primary prophylactic G-CSF treatment is recommended if the overall risk of FN for a patient is ≥20 % or between 10 % and 20 % in the presence of patient characteristics that increase the overall risk, such as age >65 years. G-CSF is an important growth factor for stimulating the recovery of bone marrow.16 G-CSF is a glycoprotein cytokine, with an approximate molecular weight of 20 kDa, which stimulates proliferation of neuropoietic progenitor cells and their subsequent differentiation to granulocytes, as well as functionally activating mature neutrophils.17
Human G-CSF is a single polypeptide chain protein, 174-amino-acidslong, with an O-glycation at one threonine residue. It binds to a specific transmembrane receptor on various haematopoietic cells, including stem cells, multipotent progenitors, myeloid-committed progenitors, neutrophils and monocytes.18 Accofil®/Grastofil® contains the active ingredient filgrastim,19,20 which is a recombinant human G-CSF produced in Escherichia coli. Filgrastim produced by E. coli is non-glycated and consists of 175 amino acids. It contains five cysteine residues, which form two disulphide bridges leaving one free cysteine residue. Accofil/ Grastofil (filgrastim) is indicated to stimulate the production of white blood cells in the following situations:19
- The reduction in the duration of neutropenia and the incidence of FN in patients treated with established cytotoxic chemotherapy for malignancy (with the exception of chronic myeloid leukaemia and myelodysplastic syndromes) and for the reduction in the duration of neutropenia in patients undergoing systematic myeloablative therapy followed by bone marrow transplantation considered to be at increased risk of prolonged severe neutropenia. The safety and efficacy of Accofil/Grastofil are similar in adults and children receiving cytotoxic chemotherapy.
- The mobilisation of peripheral blood progenitor cells (PBPCs).
- In patients, children or adults with severe congenital, cyclic or idiopathic neutropenia with an absolute neutrophil count (ANC) of ≤0.5 x 109/l, and a history of severe or recurrent infections, long-term administration of Accofil/Grastofil is indicated to increase neutrophil counts and to reduce the incidence and duration of infection-related events.
- Treatment of persistent neutropenia (ANC ≤1.0 x 109/l) in patients with advanced HIV infection, to reduce the risk of bacterial infections when other options to manage neutropenia are inappropriate. Neupogen® (manufactured and marketed by Amgen Ltd) has been in clinical use since 1991 and is the chosen reference product for Accofil/Grastofil (filgrastim).
This paper summarises the results of the Accofil/Grastofil (filgrastim) clinical programme, which was conducted to investigate biosimilarity of the investigated product with the US-licensed and EU-approved reference product, Neupogen. Two papers on the biological effects of both filgrastim products on the coagulation system have been published previously.21,22 The Accofil/Grastofil clinical programme was preceded by a preclinical programme, although this is out of the scope of this current paper.
The clinical development of the investigated product included four comparative clinical pharmacology studies in healthy adult volunteers, in which Accofil/Grastofil (filgrastim) was assessed at and around the main clinical dose (5 μg/kg) in a single and multidose setting, using both the IV and SC routes of administration, in terms of PD and PK. Efficacy and safety including assessment of the immunogenicity of the investigated product was assessed in a phase III study in cancer patients with stage IIA, IIB or IIIA breast cancer receiving chemotherapy. This publication presents the PK/PD data from healthy volunteers as well as efficacy and safety outcomes in a cancer patient population.
Patients and Methods
The Accofil/Grastofil (filgrastim) clinical programme spanned from July2007 to May 2010. Four comparative phase I studies were conducted in healthy volunteers in total (235), to compare PK and PD parameters, as outlined in Table 1: KWI-300-101, KWI-300-102, KWI-300-103 and G-CSFSUIN- 05SB0I-3FA. Simultaneous to the phase I KWI-300-101, KWI-300- 102 and KWI-300-103 studies, an additional purification step was added to the product manufacturing process of Accofil/Grastofil. Thus, the purpose of this three-arm phase I study was to bridge the existing clinical data for Accofil/Grastofil against the comparator, EU-approved Neupogen to US-licensed Neupogen by:
- Demonstrating similar PK and PD between Accofil/Grastofil and each of the active controls (US-licensed Neupogen and EUapproved Neupogen); and
- Demonstrating similar PK and PD between US-licensed Neupogen (US reference) and EU-approved Neupogen (EU reference).
In the phase III study, KWI-300-104, the safety and efficacy of Accofil/ Grastofil (filgrastim) was compared with published data for the approved reference product, Neupogen, in the reduction of the duration of neutropenia in patients with breast cancer who were undergoing chemotherapy.
Ethical committee approval for the trials was received prior to initiation of the studies and subjects were enrolled after signing informed consent forms.
Study Sites
The phase I studies KWI-300-101, KWI-300-102 and KWI-300-103 were conducted at the Department of Clinical Pharmacology at the Medical University of Vienna, Austria, and G-CSF-SUIN-05SB01-3FA was conducted in the Apotex BioClinical Department (clinic site), Toronto, Canada. The phase III clinical study KWI-300-104 was initiated across 26 sites in 11 countries. In these 17 sites in 10 countries (Austria, Bulgaria, Byelorussia, Hungary, Macedonia, Poland, Romania, Russia, Serbia and Ukraine) 120 subjects were enrolled.
Enzyme-linked Immunosorbent Assay for Antigranulocyte- colony Stimulating Factor Antibodies
Immunogenicity assessment was based on a multi-tiered approach consisting of a screening, confirmatory and neutralising assay. The analysis involved the following steps:
Step 1: Screening assay performed on all serum samples for detection of anti-filgrastim antibodies.
Step 2: Confirmatory assay performed on all samples with positive results obtained in the screening assay.
Step 3: Neutralising assay performed on confirmed positive samples to assess neutralising potential of anti-filgrastim antibodies.
Anti-drug antibodies (ADAs) were assessed using a validated enzymelinked immunosorbent assay (ELISA).23 Accofil/Grastofil was coated to 96- well plates. Quality control samples were generated by spiking goat antihuman G-CSF antibody into 10 % human serum. Goat-derived standard was used as human anti-human G-CSF antibodies are not commercially available. For detection of the animal-derived antibodies, anti-goat immunoglobulin (Ig)G-horseradish peroxidase (HRP) was used. 1:10 diluted human serum samples were detected with a polyclonal goat-anti-human IgG/A/M-HRP, thus facilitating ADA detection of IgG, IgM and IgA isotypes.
In first screening round, diluted serum samples were incubated on the plate coated with G-CSF protein. Bound anti-G-CSF antibodies were detected with goat anti-human IgG/IgA/IgM HRP-conjugated antibody based on HRP signal. The cut point was calculated by adding 1.645 x standard deviation (SD) to the mean optical density (OD) of the sample set.
The confirmatory assay was performed on all serum samples showing positive results from the screening assay. The specificity of reactive samples was assessed in a confirmatory assay based on competitive inhibition. Additionally, as part of the confirmatory assay, all samples were tested on their titre by titration to 1:15–1:60 dilution.
Results
Phase I, KWI-300-101
In total, 36 subjects were included in the intent-to-treat (ITT) population, and 35 subjects were analysed (per protocol [PP] population). The mean concentration-time profile for the test and reference items in the PP population, which points to comparability between the two products, is shown in Figure 1. In terms of the clinical PD endpoint peak concentration (Cmax) of ANC, there was no statistically significant difference between the investigated product and the reference drug, Neupogen. The mean ANC time course for Accofil/Grastofil and the reference item, Neupogen is shown in Figure 2. There was a small significant difference between investigated product and reference product in terms of the followingendpoints of filgrastim: area under the curve (AUC)0–32 (min*pg/ml) (90 % confidence interval [CI], 88.7–92.7 %), AUC0–∞ (min*pg/ml) (90 % CI 88.7– 92.7%), and Cmax (pg/ml) (90 % CI 93.6–105.8 %). In terms of the relevant CIs, however, these differences were within the pre-defined equivalence margins (i.e. 80–125 %), thereby suggesting a lack of clinically meaningful differences between the test and reference products.
A total of 59 AEs occurred during the trial, mostly classified as mild (n=40) or moderate (n=18). The numbers of subjects experiencing AEs were similar between the two treatment groups. The only severe AE (diarrhoea) occurred days after administration of the study medication and was classified as not being causally related by the investigator. The most frequent AE was musculoskeletal and connective tissue disorders with both the investigated product (n=7) and the reference product (n=6).
Phase I, KWI-300-102
The number of subjects in the ITT and PP populations was 73 and 68, respectively. In the PP population at 150 mcg dose level, the mean concentration time profile of both the investigated and reference product is shown in Figure 3 and the mean ANC time course subdivided in the test and reference item is shown in Figure 4. The predefined equivalence criteria were fulfilled for both the 75 and 150 μg dose: all PK and PD parameters met the pre-defined acceptance criteria with CIs, which were within the pre-defined equivalence limits (80 %–125 %). Furthermore, the parameters between the investigated and reference product were very similar (within narrow ± 10 % limits).
A total of 142 AEs were reported, 10 of which were experienced prior to the first injection of study medication. Of the remaining 132, most AEs were classified as mild (n=112) or moderate (n=28). Two severe AEs (one classified as related; one classified as not related) occurred after administration of the study medication. The severe AE classified as related by the investigator was an erythema at the injection site, which resolved after 1 hour and 5 minutes without intervention. Both the number and severity of AEs were similar for the investigated product group compared with the group treated with the reference product.
Phase I, KWI-300-103
Seventy-eight subjects were included in the ITT population and 75 in the PP population. Tables 2 and 3 summarise the data for the PK parameters Cmax and t1/2, respectively, for filgrastim by treatment group (PP population).
Statistical analyses are provided for PD parameter Cmax of the ANC and the PK parameters AUCss, AUC0–24, AUC0–∞ and Cmax of filgrastim in Table 4. All data fully complied with the requirements for biosimilarity in terms of the test product, Accofil/Grastofil, with the reference product Neupogen as well as the 90 % CI, which were not only within the specified statistic equivalence margins of 80–125 % for all analysed parameters, but always spanned a range including the 100 % bioequivalence reference value.
There was a similar increase in the mean CD34+ cell count and a similar inter-individual variability when comparing the test item investigated product and the reference item Neupogen after four daily doses of G-CSF. The inclusion of a placebo group allowed for a direct comparison of the cell counts, which did not substantially change from day 1 (2.34±0.70/μl) to day 5 (2.56±0.78/μl) as illustrated in Figure 5.
Mobilisation of CD34+ stem cells in the peripheral blood was analysed as a secondary PD endpoint (an indirect indicator of the marrow repopulating ability of PBPCs in line with the stipulations from the Annex to Guideline on Similar Biological Medicinal Products Containing Biotechnologyderived Proteins as Active Substance: Non-Clinical and Clinical Issues).24
There were a total of 201 AEs reported in this study, all of them nonserious and mostly classified as mild (n=154) and moderate AE (n=40). Seven AEs were classified as severe AEs (3.5 % of all AEs) and occurred after receiving the investigational medicinal product (four events in three subjects), after receiving the reference product Neupogen (two events in two subjects) and after placebo (one event in one subject). The four severe AEs after injection of the investigated product were two sequential events of headache in one subject classified as possibly related from the investigator. The most common AEs were musculoskeletal and connective tissue disorders, occurring in 27/36 (75.0 %) in the Accofil/Grastofil group 24/36 (66.7 %) in the Neupogen group and 2/6 (33.3%) in the placebo group.
Phase I, G-CSF-SUIN-05SB01-3FA
Forty-eight subjects were dosed in the study and completed the first period of the study. Forty-five subjects completed at least two periods of the study and, of these, 40 subjects completed all three periods of the study. Consequently, the safety population included all 48 randomised subjects since all subjects received at least one administration of the study treatment. The PK/PD dataset included 45 subjects, which is in accordance with the protocol that defined the PK/PD population as subjects who completed at least two periods of the study.
Mean ANC concentration time profiles obtained after the single subcutaneous administrations of Accofil/Grastofil, EU-approved Neupogen and US-licensed Neupogen are presented in linear and log plots in Figure 6A and B. Average concentration-time profiles obtained by plotting mean concentration-time values for all subjects included in the PK/statistical analysis, are presented on both linear-linear and log-linear scale in Figures 7A and B, respectively. PD results of Accofil/ Grastofil Filgrastim versus EU-approved Neupogen and versus USlicensed Neupogen are shown in Table 5.
There were 347 AEs reported by subjects in this study, the most common AEs probably related to the PD of filgrastim were transient early decreased neutrophil counts. In total, 108 events of decreased neutrophil count were observed in 45 out of 48 subjects (93.8 %). No difference was noted between treatment arms for the events of decreased neutrophil count. Additionally, there was no evidence of anti-drug antibody formation in this study. Overall, a very small percentage of samples collected for the assessment of immunogenicity were positive in the screening assay over the course of the study (ie. eight samples out of 185 samples with similar distribution between treatment arms). None of these samples were confirmed to be positive in the confirmatory assay. This indicates therefore that the administration of the filgrastim preparations did not result in an immunogenic response. There were no reports of death or serious AEs.
Phase III, KWI-300-104
This patient population consisted of 120 Caucasian female patients of mean age 50.0 years (SD 9.5 years), with stage IIA, IIB or IIIA breast cancer without neoadjuvant chemotherapy for this breast cancer. There were 39 (32.50 %) patients at tumour stage IIA, 44 (36.67 %) at stage IIB and 37 (30.83 %) at stage IIIA. The main efficacy endpoint, the mean (SD) duration of severe neutropenia in cycle 1 (defined as an occurrence of ANC <0.5 × 109/l), was 1.40 days (±1.07 days). The frequency of severe neutropenia in cycle 1 was 93 (77.50 %).
The mean ANC nadir of 0.37 x 109/L was recorded on mean (SD) day 7.20 (0.64). Post-nadir ANC >1.5 x 109/l, relative to chemotherapy administration, occurred after a median of 9 and mean (SD) 9.11 (1.32) days. The mean CD34+ compared with mean ANC values in the full analysis set is shown in Figure 8. It was not possible to measure consistently the duration of neutropenia in consecutive cycles2–7 due to lower frequency of blood sampling. CD34+ cell counts were performed at selected sites and for a total of 39 randomly selected patients. Three samples were taken from patients in cycle 1. An increase over baseline was observed in mean and median values at days 7 and 9. Mobilisation of CD34+ cells was demonstrated by rise to mean (SD) 14.49 (28.82) x 106/l at cycle 1 day 7 and to 110.67 (101.18) x 106/l at cycle 1 day 9, over 4.57 (3.33) x 106/l at cycle 1 day 1.
Most AEs were described as mild in severity (748 events, 61.51 %). AEs were described as moderate in 368 (30.26 %), severe in 99 (88.14 %) and life threatening in one (0.08 %) case. The one life-threatening AE was polyorganic insufficiency due to disease progression and this was not deemed related to treatment. The most frequently reported AE was bone pain, which was reported 267 times by 80 (66.67 %) patients. It was most frequently described as mild in 105 (39.33 %), moderate in 99 (37.08 %) and severe in 63 (23.60 %) cases.
Discussion
The EMA evaluated that similarity has been convincingly demonstrated between Accofil/Grastofil at and around the main clinical dose (5 μg/ kg) and the reference product, Neupogen.25 In the Annex Guideline on Similar Biological Medicinal Products Containing Biotechnology-Derived Proteins As Active Substance: Non-Clinical and Clinical Issues, robust PD data are considered pivotal in the demonstration of biosimilarity.3 The data supporting the high similarity between the filgrastim biosimilars are further substantiated by extensive analytical and bioactivity assay comparisons.26 The main efficacy endpoint of the phase III study KWI- 300-104 was the duration of severe neutropenia in cycle 1 (defined asoccurrence of ANC below 0.5 x 109/l). The mean (SD) duration of severe neutropenia in cycle 1 was 1.40 (1.07) days, which is in line with the reports in published literature.27 Cycle 1 sampling for ANC was robust as this was the most relevant and sensitive cycle for assessment of the efficacy as measured by the duration of severe neutropenia. This finding is supported by published literature.28
The mechanism of action of G-CSF is at the receptor level.29 Consistent with the mechanism of action of filgrastim on ANC, the mechanism of action of filgrastim on PBPCs mobilisation is the same in healthy subjects and in patients and this is supported by its clinical use in both healthy stem cell donors and in cancer patients.16 Several studies reported in the literature have assessed various dose and dosage regimens with filgrastim in relation to the achievement of optimal PBPC mobilisation and hence CD34+ yield.30–32 Hence, the overall high intra-individual variability in both responding to treatment and in the mobilisation of stem cells, clearly suggests that in clinical practice the dosing regimen with filgrastim will need to be individualised such that the treatment with filgrastim for the mobilisation of PBPCs will ultimately be driven by the patient response. These outcomes reported herein are similar to those from the filgrastim arms of the reference studies by Green et al.33 and Holmes et al.34 Both these studies were performed in the same indication and with similar filgrastim dosing regimens. However, baseline characteristics and differences in protocol procedures do not allow direct comparisons of the studies.
The extent of mobilisation, taking into consideration the pathological confounders as well as innate inter-individual variability, is ascertained through evaluation of the individual’s white blood cell count, or measurement of peripheral blood CD34+ count. This underscoresthe variability that can be observed, and the need to apply clinical decision-making when dealing with patients. Broad inter-individualvariation in the capacity of patients to mobilise progenitor cells was noted in the phase III study, a finding that is consistent with the reported literature.16,24
There are no new adverse reactions observed with Accofil/Grastofil(filgrastim) that differ from what has been described previously with Neupogen.25 The CHMP considered that the overall safety profile of the product is acceptable. Adverse effects seen with filgrastim treatment include headache and diarrhoea reported shortly after starting filgrastim therapy, typically in less than 10 % of patients. An initial transient decrease in the number of circulating neutrophils after intravenous or subcutaneous filgrastim injection has been reported previously.35–38 These initial decreases were consistently followed by rapid and significant increases in neutrophil count within 4–6 hours. The mechanism of the early depression is thought to be due to margination of neutrophils to endothelial cells.39 The incidence of immunogenicity is expected to be low, and this risk is addressed in the risk management plan.40
In accordance with the published information and the prescribing information, splenomegaly is a known identified risk of GCSFs such as Neupogen.41 No patients had a diagnosis of hypersplenism and no patients underwent splenectomy.
Additional pharmacovigilance activities post-authorisation are currently being undertaken for Accofil/Grastofil, including reporting and discussion of all identified and potential risks, and reviews of serious and longterm AEs from registries. Several studies of G-CSF treatment of normal aphaeresis donors have been published. A summary of the doses used and AEs reported for approximately 400 normal subjects treated at various institutions worldwide is shown in Table 6. Musculoskeletal bone pain is the most frequently reported AE, as observed during the Accofil/Grastofil (filgrastim) clinical programme. In the phase I studies, the AE profiles, including that for bone pain, were similar between the Accofil/Grastofil and Neupogen groups. The high rate of bone pain observed in patients in the phase III study may have been as a result of the way in which it was reported: patients assessed their own bone pain severity and incidence and muscle pain, back pain and neck pain was all recorded as bone pain. In support of this, the AE profile in terms of bone pain was similar between Accofil/Grastofil and Neupogen in the phase I studies suggesting that in a clinical setting the incidence of bone pain should be similar between Accofil/Grastofil and Neupogen.
In summary, the efficacy and safety results, taken together with the PK and PD data from the phase I studies, demonstrate the biosimilarity of Accofil/Grastofil and Neupogen.